A posterior cruciate ligament (PCL) tear is an injury in the back of your knee, which can cause pain, instability, and difficulty walking or participating in physical activities. While it’s less common than other types of knee ligament injuries, like an ACL tear or a LCL tear, it still can limit your ability to move.
PCL anatomy
The PCL is the strongest knee ligament and is made up of two parts: anterolateral and posteromedial bands. Like all ligaments, these bundles of fibrous tissues have a poor blood supply, which makes injuries to the PCL longer and more difficult to heal than most structures.
The PCL originates from the side and front of the medial condyle of the femur at the intercondylar fossa (the notch of the thigh bone that gives its familiar shape) and inserts into the back of the tibia’s flat surface.
Detailed image of the PCL and posterior knee
Its job is to prevent the femur from sliding horizontally across the tibia and limit excessive abduction (varus) and adduction (valgus) of the knee.
PCL tear causes
Trauma to the knee is a common cause of a PCL tear. This can happen from an impact to the shin bone near the knee while it is flexed. One 2003 study of nearly 500 patients found that about 45% of the PCL tear is caused by a vehicle accident and 40% are caused by athletic injuries. About 28% of these accidents are from motorcycles and 25% of the athletic injuries are from soccer.
Although non-contact injuries are low, it can still happen among certain populations. One Norwegian case-control study of 104 patients with a PCL tear found that those who had a non-contact injury had a steeper slope on the top of their tibia compared to the control group, potentially raising the chance of a PCL tear when the knee twists sharply during hyperextension.
How common are PCL tears?
While an isolated PCL tear is less common than other types of knee pain and injuries, the frequency depends on the population.
- In professional American football, about 3% of 2,285 players of the NFL Combine (2009-2015) were found to have a PCL tear during the pre-draft, even if they had no symptoms.
- In one county in Minnesota, there were about 1.8 complete PCL tears per 100,000 people, with more among young men aged 20 to 49.
- PCL tears make up 0.65%–3% of all sports-related knee injuries in the U.S. and Europe.
- A Scandinavian study found that isolated PCL tears occurred among more than one-third of the total number of PCL injuries. Soccer players ranked as the highest prevalence among all sports (13.1%).
Image of a dissection of the posterior knee
PCL tear symptoms
Symptoms may overlap with other causes, like hamstring strain or a Baker’s cyst, or other types of pain behind the knee. Symptoms include:
- Swelling behind the knee
- Achy pain
- Dull pain during movement
- Instability in the knee, which may feel “looser” than normal
PCL injuries can occur with other types of knee injuries, such as torn knee meniscus, osteoarthritis, and—in rare instances—ACL tears. Thus, each person may have different symptoms of posterior knee pain because of a combination of different causes.
PCL tear diagnosis
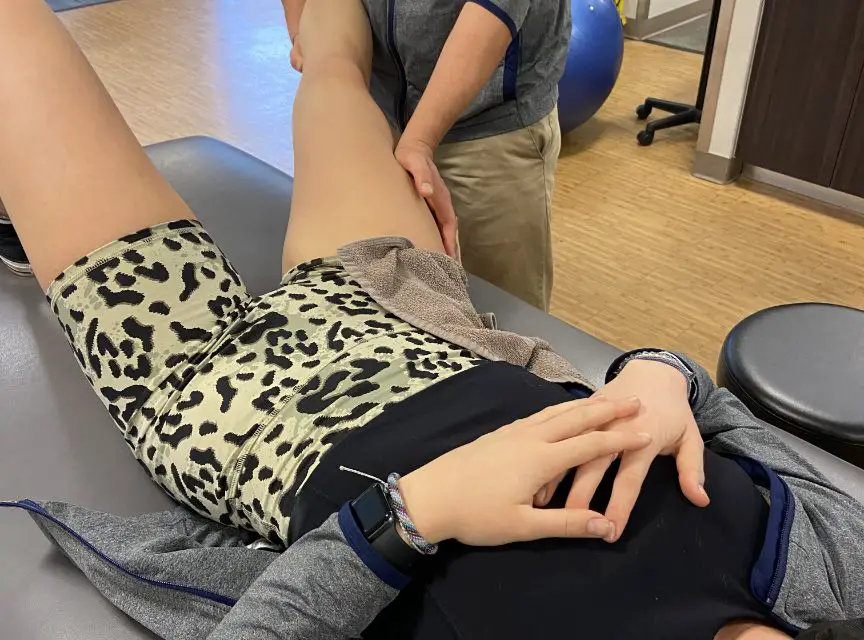
A PCL tear or injury may require different testing, depending on the symptoms and the nature of the injury. It can be challenging for clinicians to diagnose because there may be one or more causes of pain besides the PCL injury.
Posterior drawer test
One common test that a clinician might use is the posterior drawer test, which has a high sensitivity rate of 90%. This means that it has a high accuracy rating of identifying a PCL tear.
During the posterior drawer test, a clinician would:
- Have you lie on your back on the examination table
- Flex your hip at about 45 degrees and your knee flexed at 90 degrees.
- Push sharply at the tibia near your knee joint while the femur is stabilized.
If there is a PCL tear, the tibia would slide horizontally relative to the femur. The amount of movement would depend on the grade of the tear:
- 0 to 5 millimeters for grade 1
- 6 to 10 millimeters for grade 2
- 11-plus millimeters for grade 3
Clancy sign
The Clancy sign assesses for a PCL tear. In this test, you lie on your back with your knee bent at a 90-degree angle, and the clinician applies pressure to the tibia while feeling for abnormal movement or laxity of the knee, which may indicate a PCL tear.
Named after Dr. William Clancy, Jr., of the University of Wisconsin in the early 1980s, a positive result of the Clancy sign may indicate that the clinician cannot feel the bony projections to either side of the tibial plateau beneath the femur’s condyles.
A positive Clancy sign means the normal bumps on the tibia (on the tibial plateau) are not felt when the knee is bent to 90 degrees. This indicates that there may be a PCL tear.
Dial test
The dial test is used to assess rotational instability in the knee and help diagnose injuries to the PCL and posterolateral corner (PLC) of the knee. In this test, the clinician would:
- Have you lie on your stomach on the examination table with your hips and knees bent at 90 degrees.
- Place one hand on the back of your thigh to keep your upper leg in place.
- Rotate your ankle and foot externally.
During the dial test, the patient lies on their back with the hips and knees bent to 90 degrees. The examiner then rotates the foot to see how much the tibia can turn outward.
A positive dial test, meaning increased outward rotation of the injured tibia compared to the uninjured side, can indicate a few different things:
- If there’s more than 10 degrees of external rotation compared to the other uninjured knee, then there might be a PCL injury. An intact PCL typically limits rotation at 90 degrees.
- Contrary to previous understanding, most patients with only a PLC injury actually have a positive dial test at both 30 and 90 degrees, not just at 30 degrees.
- The dial test alone cannot reliably distinguish between these different knee injury patterns. It should be used with other tests of the PCL and medial ligaments to make an accurate diagnosis.
Chahla et al. cited that if the same test was done with the leg flexed at 90 degrees and there is a greater external rotation, then there might also be injury to the posterolateral complex of the knee (PLC). This area includes—but not exclusively—the popliteus tendon and muscle, lateral collateral ligament, popliteal ligament, and the biceps femoris.
The sensitivity of the dial test, however, may not be reliable. A cadaver study from South Korea found that it may not be able to detect injury to one or two posterior knee structures. The researchers suggested that “comprehensive diagnostic methods” should be used with various knee tests, including patients’ history, physical examinations, radiographs, and magnetic resonance imaging.
Reverse pivot-shift test
The reverse pivot-shift test checks for damage to the PCL by looking for unusual movement of the tibia compared to the femur when the knee is bent. It has a low sensitivity rate of 26% and a high specificity rate of 95%, which means that it’s not very accurate in correctly identifying people with a disease or injury but it’s very accurate in identifying those without a disease or injury.
In a reverse pivot-shift test, a clinician would
- Flex your knee to 90 degrees while you’re lying on your back on the examination table.
- Extend your knee while applying pressure to abduct your knee and externally rotate your foot.
In a positive test, the tibia plateau is partially “out” of the knee as the knee flexion is reduced between 20 to 30 degrees. The clinician should not compare your affected leg with the opposite leg.
Posterior sag test
The posterior sag test (or Godfrey test) assesses for a possible PCL tear by observing for a posterior sag of the tibia when the patient lies supine with their hips and knees flexed to 90 degrees.
The clinician checks your injured leg to see if there’s too much inward curving at the top of the tibia near the knee. Normally, there should be a small protrusion of the tibial plateau below the knee joint. If there is none, it’s likely a sign of a PCL tear.
PCL tear treatments
The type of PCL treatment you get depends on various factors, such as whether the symptoms are acute or chronic, the severity of the tear, or if the injury is at the PCL only or if there are injuries at other parts of the knee.
Surgery
Surgery is used to restore stability and knee function by repairing or reconstructing the damaged PCL.
A 2018 review cited several studies that partial PCL tears (grade 1 and 2) have mixed results in outcome from conservative treatments, such as exercise and knee bracing, while surgery repairs of full PCL tears are recommended. However, there is still a debate on which type of surgery is better than another.
“Most authors agree that partial isolated PCL tears should be treated nonoperatively,” the review authors Pache et al. wrote. “Complete PCL tears treated nonoperatively have been reported to increase the risk of degenerative changes of the medial and patellofemoral compartments at long term, and were associated with poor function.”
They also noted that there has not been any long-term research on whether a PCL reconstruction surgery can prevent the onset of knee osteoarthritis.
A nationwide Taiwanese study that was published in 2018 favors surgical interventions over non-surgical ones. Researchers from the National Defense Medical Center in Taipei reviewed nearly 4,200 diagnoses of PCL tears from 2000 to 2015. They found that those who had surgery were less likely to get knee osteoarthritis, total knee replacement, and meniscus tear than those who had conservative care. Overall, the researchers cited several studies that show many patients recover within two to five years.
“These results raise concerns regarding the need to restore stability with PCL reconstruction to avoid progressive degeneration,” they wrote.
Some research they cited include:
- A 2006 South Korean study, subjective evaluations reported that all 61 patients (45 men, 16 women) were “normal or near normal” while objective evaluations reported all but two patients as “normal or near normal.”
- In a 2009 Belgian study that followed up with 25 patients (22 men, 3 women) who had a PCL reconstruction surgery in 1995 to 2001, 75% of them tended to have more damage to the knee cartilage than those who had a reconstruction within one year.
However, Taiwanese researchers from the review pointed out that the data they used were claims-based, meaning that the information was sorted from insurance companies, doctor’s offices and bills, and other similar paperwork. They do not inform the researchers the degree of the PCL tear or the severity of the other knee symptoms.
Even those conservative treatments may underscore surgeries for a torn PCL, they still have their place in the treatment spectrum. If the PCL tear is an isolated incident and is acute, then non-operative treatments may be a better option for some patients.
A 2007 study in New York City in 2007 found that there was no pain among 38 out of 58 knees examined (57 patients total), while there was mild pain among 14 knees and moderate pain among 6 knees. About 91% of the patients had swelling in the knee.
The researchers reported that only two patients failed conservative treatment because of “clinical deterioration of symptoms” and had reconstruction surgery. They were able to return to play their favorite sports where one had a 38-month follow-up while the other patient had a follow-up nearly eight years later.
Another study in Indianapolis, Indiana, in 2013 followed up with 68 patients who had conservative care for their acute PCL tear. Although 11% of them had developed knee osteoarthritis, all of the patients were “active, have good strength and full knee range of motion, and report good subjective scores.”
Like most types of knee pain, treatment for a PCl tear or injury should be tailored to the individual, including how clinicians communicate to the patient. Considering that pain is biopsychosocial in nature, and a PCL tear itself is biological, how patients perceive their injury, what it means to them, and how the healthcare infrastructure on how well patients get treated all play important roles in pain and disability outcomes.
Massage therapy and PCL tear
Massage therapy can alleviate the pain and stiffness temporarily for a PCL tear as well as other types of knee pain. While there isn’t a specific technique or recipe for a PCL tear, registered massage therapist Rob Haddow suggests that therapists should focus on the individual patient’s problem and condition first.
“There’s no panacea. It’s an injury, not a recipe,” Haddow said. “When we talk about massage protocols for various ligaments—PCL included—we’ll often find dogmatic approaches suggesting treating the body as a zigzag of tight and weak structures alternating up a kinetic chain. While that approach isn’t necessarily without merit, it is far from enough to base a treatment around.”
Haddow said that two patients who have the same injury does not mean that they will experience pain and movement the same way. Thus, massage therapists need “a solid assessment strategy” rather than assumptions based on what they had learned in their schooling.
“Our treatment plan should once again, be built on a solid series of assessments, and our remedial exercises and home care should reflect a relevant troubleshooting approach,” Haddow said. “Goals need to be reasonable and attainable, but should also invite feedback from our patients and help to address any concerns.”
“Rather than walking into a treatment plan with expectations, we (massage therapists) should approach it with a detective mindset,” Haddow continued. “Instead of assuming something about the state of the body based on a special test, we should approach recovery from a state of reducing pain and building tolerance. We should allow our patient to tell us what they are experiencing and work with that, not telling them that they will be in pain and ‘dysfunctional.’”
Further reading
How Central Sensitization Affects Chronic Pain
How Massage Can Help Treat Chronic Pain
What Is Pain and Why Do We Feel It?
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.