Hip pain comes in a garden-variety like shoulder pain, knee pain, and back pain. And so, there’s no one-size-fits-all treatment for it. Sometimes different types of hip pain overlap with one another, like hip flexor pain with snapping hip syndrome. And sometimes pelvic pain, such as endometriosis and pelvic inflammatory disease, can have similar symptoms that can be mistaken for one or another.
This makes diagnosis tough for many clinicians, and treatments could be a trial-and-error process, which can be costly and painful—physically and emotionally.
Instead of blaming a “tight” muscle, a pinched nerve, osteoarthritis, and a ton of other factors that may cause hip pain, an in-depth look at some of the common causes can help you decide which is the best route to your condition.
Massage therapy may help alleviate some pain and help you move better in the short-term, but some types of hip pain may require the therapist to approach each case uniquely. And so, your therapist shouldn’t be doing a cookie-cutter treatment.
What causes hip pain that radiates down the leg?
There are a few things that can cause pain radiating down the leg. Milligan said that if the pain is mostly in the back of your leg, the first thing to make sure is that the pain isn’t coming from the spine because clinicians could be missing something if they’re just addressing the hip.
“Rule out nerve irritation or radiating back pain from the lumbar spine,” said Dr. Mark Milligan, who is a physical therapist at Vori Health and director of CEO of Anywhere Healthcare. “Soft tissues around the hip may radiate down the leg. If there’s too much load demand from the glute muscles, that may cause radiating posterior leg pain. Every time you step, it could be hip pain from your gluteus minimus or glute medius.”
To pinpoint exactly what you may have, your healthcare professional will likely rule out more common and serious conditions while reviewing your health and lifestyle history.
Some types of hip pain stem from the hip joint where inflammation occurs, or it could be an irritated nerve deep in your buttocks. In some cases, hip pain can travel down your leg and foot (or vice versa) where the symptoms manifest.
“I like to break hip pain down based on where the patient points to their pain, where they describe their pain, and what structures are in that area or referred to that area,” said Milligan. “I take into consideration their age, activity level, their ‘why’ and ‘how’ it started.”
Milligan said that 90% of the information clinicians get from their patients comes from the patients’ description. “You get a ton of information by doing a thorough subjective history of that patient,” he said. “When you think about where the patient feels the pain and the structures that surround that area and refer to that area can give you a better idea of what’s happening. It could be ‘deep’ in their hip or radiating down their leg.”
Osteoarthritis is the most common source of pain, at least in Milligan’s experience. Anterior hip impingement and labral could be a cause of front hip pain, and that type of pain can radiate down to the knee.
Degenerative changes in the hip joints are “totally normal.” “It’s just a matter of whether they’re painful or not,” he said.
Femoroacetabular Impingement (FAI)
Femoroacetabular impingement syndrome is an abnormal contact between the round head of the femur (thigh bone) and the pelvis’s socket (acetabulum). This can lead to microtrauma to the joint, damaging various joint structures, which may lead to hip osteoarthritis.
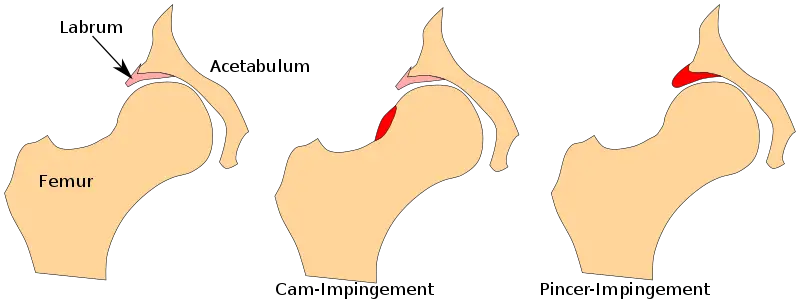
Image: OpenStax College – Anatomy & Physiology.
It may also lead to damage to the labrum—the cartilage that reduces friction between the femur’s head and the socket—which may lead to hip pain and inflammation to the hip joint.
While it tends to happen among active, younger people (e.g. athletes), FAI can also occur among older adults, oftentimes with no symptoms.
Gluteal tendinopathy
This condition used to be called “gluteal amnesia,” a term that Dr. Stuart McGill coined. It’s the inability to engage the hips during exercise which may negatively affect athletic performance and increase the risk of injury. But current scientific evidence does not support this idea of your butt having such “amnesia.”
Photo: Penny Goldberg
Gluteal tendinopathy is a broad term that includes pain and inflammation of the tendons of the gluteus medius and minimus. It often occurs in older people, particularly among women in their forties to sixties and higher.
Pain from gluteal tendinopathy usually occurs in the lateral hip area by the greater trochanter of the femur. Similar to hip arthritis, gluteal tendinopathy can start as a subtle, nagging pain that gradually worsens over time.
Sciatica
Sciatica is the radiating pain that often “shoots” down the leg and sometimes into the heel of the foot. While it tends to affect one side of the body, sciatica is sometimes caused by the irritation of the sciatic nerve in one side of the hip.

Photo: Halley Moore
Oftentimes, the piriformis muscle is to blame, but there are multiple causes of sciatica where some of them are less obvious.
Sometimes the pain can last for days or weeks, and sometimes it “happens” without warning. But the good news is: sciatica does go away on its own most of the time.
Piriformis syndrome
The symptoms of piriformis syndrome are similar to sciatica. Unlike sciatica, this condition is often not associated with spinal problems. Patients with piriformis syndrome typically report deep pain in the buttocks that may radiate down into the back thigh.
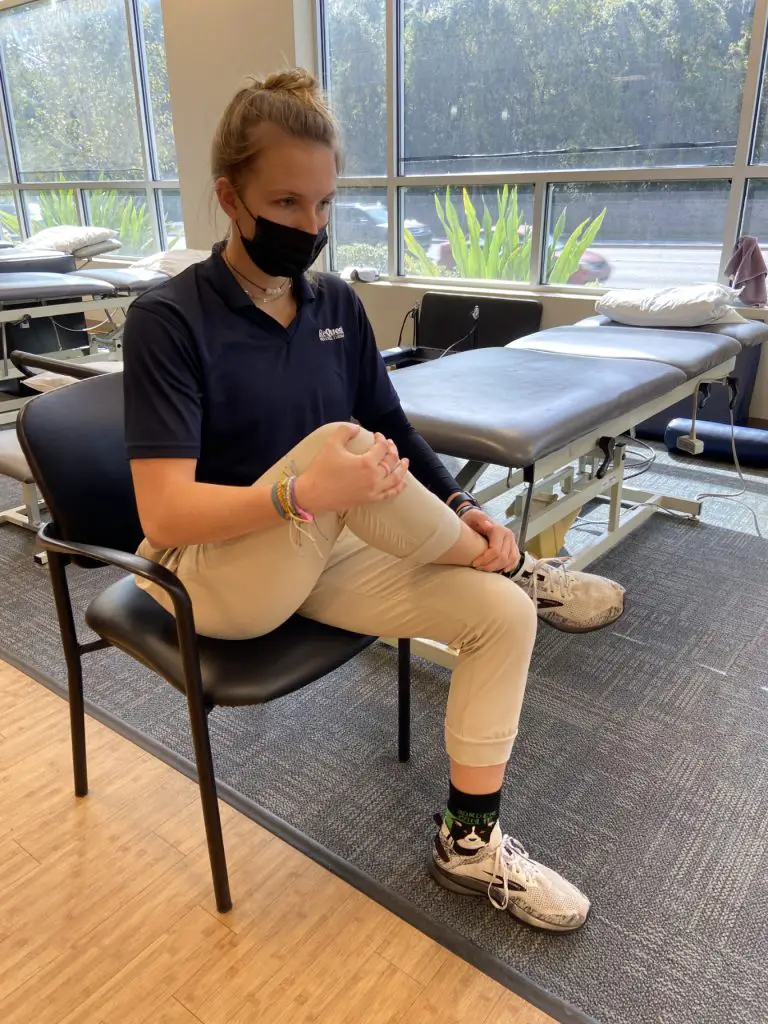
Seated piriformis stretch, knee to shoulder. Photo: Penny Goldberg.
While many case of this condition tend to be from the irritation of the sciatic nerve against the piriformis muscle, not every case may stem from this cause because some people may have different branching of the sciatic nerve in relation to the piriformis and other gluteal muscles.
Hip flexor pain
Compared to other types of hip pain, there is less research about hip flexor pain, which makes it difficult to diagnose and treat. Sometimes the pain is not from the psoas or iliacus but from visceral pain, such as appendicitis and diverticulitis.

Photo: Fábio Ericeira
Symptoms of hip flexor pain overlap with other types of groin pain, which can be mistaken for pain in the psoas. Treating the psoas alone may not be the right way to do so since these muscles lie deep from the skin. Thus, “digging” deep into the muscle can be uncomfortable for many people and may worsen their hip pain.
Iliotibial band syndrome
Too much friction between the iliotibial band (IT band) and the lateral knee or the thigh muscles are often blamed for iliotibial band syndrome. This usually happens to those who engage in prolonged repetitive movements in the legs, such as runners and cyclists.

Photo: Tania Dimas
While many massage therapists suggest that the IT band should be massaged and “softened,” pain research and current understanding of the IT band suggest that “deep tissue” work may not be the answer, but there are alternatives to alleviate IT band syndrome. ‘’
Sacroiliac joint pain
Sacroiliac joint pain (SI joint) can often feel like low back pain or an achy hip pain in the upper buttocks, and some researchers think that it’s underdiagnosed and undertreated.
Many narratives about the SI joint and how to treat it are more than ten years behind current research, such as having an “unstable” SI joint can contribute to hip pain or a therapist being able to “feel” a subtle tilt of the joint. But these claims aren’t supported by scientific evidence.
Leg-length discrepancy
Leg-length discrepancy is divided into anatomical and functional, where the “anatomical” refers to the physical differences of leg length while “functional” refers to movement patterns that cause the shortening of one limb.
Photo: Pixabay
Having an uneven leg length is thought to be a cause of hip pain and back pain, but some research finds that there’s little to no relationship between leg length and pain.
Like most kinds of pain, it often stems from multiple factors rather than just one cause of pain that many manual therapists tend to believe.
Treatment
Treatments for hip pain encompass a variety of approaches, ranging from non-surgical methods like physical therapy and medication to surgical interventions. Like most types of joint pain, the treatment depends on the type, underlying causes, and pain severity.
Stretching
Stretching might work for some types of hip pain, but the current scientific evidence is iffy and scarce. Any conclusion is almost as accurate as predicting a coin toss.
Piriformis syndrome stretching
Piriformis stretching intends to relieve tension and improve flexibility in the piriformis muscle and buttocks, which may alleviate pain and discomfort in the hip and lower back.
A 2020 study from Pakistan compared post-facilitation stretching—a type of muscle energy technique (MET) that uses a muscle’s stored energy to elongate its tissues—with another type of stretching called the ELODA Method, an osteopathic technique that’s based on myofascial stretching.
Based on their sample of 40 people (ages 30 to 70) who were diagnosed with piriformis syndrome, the researchers found that both stretching types reduced hip pain, but the post-facilitation group reported to have higher pain reduction than the ELODA group.
Another study on 33 ballet dancers found that “vibration-assisted” stretching to be somewhat better than MET stretching and static stretching for increasing the dancers’ pain-pressure threshold at their thighs.
But the researchers pointed out that all three types of stretching provided such short-term effects and doubted that this study can be extrapolated to other populations. Whether this has any significance to other types of hip pain is questionable.
Keep in mind that one study doesn’t automatically validate that one type of stretching is “better” than another. Many more studies are needed to determine what’s more likely to work and whether there are other confounding factors that influence patients’ outcome that have little or nothing to do with the stretching technique.
Low back pain
Stretching your hips may alleviate some low back pain, but current research has mixed results. While a 2012 systematic review found that MET stretching may be beneficial for those with chronic low back pain, a 2015 Cochrane Review found that the majority of the studies included are “poor” and have a “high risk of bias.” The authors do not find “sufficient evidence” for MET to be effective for low back pain.
Further reading: Cochrane Review Finds Lack of Effectiveness in Muscle Energy Technique
Slump stretching
Slump stretching is based on the slump test that physical therapists use to gauge how sensitive your neural and other tissues are in your spinal cord for back pain.
When you do a slump stretch, with your hands behind your back, you flex your upper and lower spine as much as you can. If that doesn’t cause any pain, you flex your neck as much as you can while extending one leg and keeping your spine flexed.
Some clinicians found some positive results with the test that they made it an exercise for their patients to treat low back pain.
While a 2019 systematic review found that slump stretching “clinically important” for back pain, the collective studies have too much variability among the test subjects and “inconsistency” and “imprecision” of how the studies were set up.
Exercise
While exercise in general has been shown to help reduce back pain and disability, there’s some evidence that it can help with some types of hip pain.
For knee and hip osteoarthritis, a 2019 systematic review found that exercise is “superior” to usual care (e.g. usual everyday activity, doctor follow up, no exercise intervention) for up to eight weeks. After that timeframe, there’s not much difference between them.
People with hip replacement may also benefit from exercise, according to another systematic review that’s based on 10 trials. The researchers found that strength training improves walking speed better than doing non-strength exercises.
However, some limitations include short-term follow-ups, limited number of studies, different patient demographics, and different experimental setup.
Whether these studies can be extrapolated to other types of hip pain is questionable, and again, this may likely boil down to the individual level with no one-size-fits all treatment.

“People who have been having symptoms for years have something that has not been addressed. They go through this list and nobody has helped them. I don’t think more manual therapy is going to help,” said Dr. Mark Milligan. Photo courtesy of Mark Milligan.
Psychological factors
Sometimes psychological factors may contribute to hip pain besides joints and muscles. Milligan recalled a patient who couldn’t move her shoulder, and her previous therapists thought she had a massive rotator cuff tear or advanced stages of frozen shoulder. Her shoulder couldn’t be moved within its full range of motion passively
“I saw her a couple of times to see how she was progressing,” Milligan said. “We talked a little bit about her stress. She wasn’t able to find a job, rent was coming up, and things like that.”
But at the last session, something changed in her.
“She walked in and was like, ‘All right, Mark, I’m ready to go!’ She lifted her arm up and waved it around like nothing ever happened,” Milligan said. “I was mystified and we started talking. What did you change? What did you do?
“And she said, ‘Mark, I got a job!’”
Milligan speculated that the decrease of her cortisol and stress in her life had also decreased her pain sensitivity. “She was discharged that day. There were no issues with her shoulder,” he said. “Pain that lingers beyond the typical tissue healing time frame should be looked beyond the physical body.”
The location of your hip pain can be a start in finding out the nature of your pain, and sometimes—as described in the types of pain earlier—the source of your pain could be from somewhere else other than the symptomatic area.
“If patients point to their posterior or buttocks, that can be a number of things like [pain] referred from the lumbar spine, hip osteoarthritis, irritation of the tissue of the posterior hip like piriformis syndrome, or external rotator with a load demand that’s too high, or it could be a neural issue,” Milligan said. “People who have been having symptoms for years have something that has not been addressed. If somebody sits in front of me and says, ‘You know, I’ve seen four PTs, three chiros, two [whatever],’ and they go through this list and nobody has helped them, I don’t think more manual therapy is going to help. Something’s missing that no one’s addressing.”
Researchers are still looking for that missing piece or pieces. As Milligan said, perhaps where clinicians and researchers should look into factors of hip pain and other types of pain beyond the biological factors, such as in the case of his patient with shoulder pain.
Perhaps one of those missing pieces for clinicians is being a good communicator—and listener—to those in pain. And no Level 1 or 2 class is going to teach anyone that.
As always, consult with your healthcare provider for the best treatment and your personal guidance. Do not use this article as a substitute for your healthcare providers’ advice.
Further reading: Does Narrative Medicine Have a Place in Massage Therapy?
Thinking about my original metaphor for pain, the rising flood, makes me want to use it more consciously. When pain comes again — my own, or someone else’s — instead of patching the dam, I might try listening to the water flow. ~ Cameron Walker, The New York Times
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.