Shoulder impingement describes the painful condition caused by decreased space between the acromion process of the scapula (the pointy, bony end of the shoulder) and the humeral head of the upper arm bone. This is called the subacromial space.
For years, shoulder impingement syndrome has been a stand-alone diagnosis when, in reality, it’s a symptom of something else. The subacromial space does not shrink on its own; something has to cause the narrowing. Finding the root cause of impingement is vital to developing an appropriate treatment plan.
Shoulder anatomy
We often hear the “golf ball on a tee” analogy used to describe the relationship of the humerus to the glenoid fossa of the scapula in the shoulder. The position of the humeral head is maintained by the rotator cuff muscles.
There’s an extra layer of movement protection afforded by the “roof” of the joint created by the acromion, coracoacromial ligament, and the coracoid process (also of the scapula). The space between the roof and the humeral head is the subacromial space.
The subacromial space is home to the subacromial bursa and rotator cuff tendons. The insertion of the long head of the biceps tendon is close to this space, but not technically in it.
In shoulder impingement syndrome, raising the arm compresses the structures in the space between the humeral head and the acromion.
Shoulder elevation is created by the interaction of the rotator cuff and stabilizing shoulder muscles as they work to keep the bony anatomy from hitting or rubbing.
The rotator cuffs are well-known for their role in throwing, but arguably, their more important job is to maintain the position of the humeral head on the glenoid as it moves beneath the acromion.
Although there can be some variation in the ratio, it’s widely accepted that there’s about a 2-to-1 relationship between the humerus and scapula during elevation. This is called scapulohumeral rhythm.
Rather than focusing on the numbers, it may be more important to simply recognize that the scapula is quiet during the start of elevation, moves in coordination with the humerus through the mid-range of motion, and then becomes somewhat stable again at angles above 90 degrees.
On the back side, the scapular stabilizers work in force couples to control movement. The upper trapezius, lower trapezius, and serratus anterior are responsible for upward rotation, while the rhomboids, levator scapulae, and pectoralis minor control downward rotation.
With the proper scapular position comes maximal acromiohumeral distance, which is the measurement used to assess the subacromial space. This space is further calculated by the occupation ratio percentage, which considers the thickness of the supraspinatus tendon or subacromial bursa.
Larger acromiohumeral distance and smaller occupation ratio mean more free space during movement and less likelihood of impingement occurring.
Illustration of shoulder impingement.
Types of shoulder impingement
Traditionally, subacromial impingement has been used to describe mechanical encroachment of the structures that live in the subacromial space.
Mechanical encroachment is where normal shoulder anatomy “invade” of the subacromial space. This occurs during the mid-range of motion and may create a “painful arc.”
Subacromial, or external, impingement is the most common type. This is where something external is causing the problem. This condition is also known as swimmer’s shoulder because of the constant repetition swimming entails. Subacromial impingement is further divided into primary and secondary categories.
- Primary external impingement is where structural changes decrease the subacromial space. Osteophyte formation, variants in acromion type, or an increase in the size of soft tissues can all narrow the space.
- Mechanical impingement is the compression or shear forces to soft tissues. In these cases, it is either a bone or ligament that is impinging on another soft tissue and creating pathological changes.
- Secondary external impingement is where muscles imbalances or tissue tightness can change movement patterns of the shoulder by changing the humeral head’s position.In these cases, the humeral head moves upward, which decreases the space and compresses the soft tissues.
External impingement
People with primary external impingement may not improve when mobility, strength, or proprioception are addressed because the fundamental cause of the problem is unchanged. Therefore, working on surrounding tissues can be an effective management strategy.
In a secondary external impingement, dysfunctional movement is the root cause of tissue compression. Repetitive actions, overuse, posture, imbalances in strength or flexibility, or poor proprioception are all possible causes.
Internal impingement
Internal (posterior) impingement, refers to a specific condition where the undersurface of the rotator cuff tendons are trapped between their attachment on the humerus and the posterior edge of the glenoid.
Entrapment occurs when the arm is in 90 degrees of shoulder abduction and external rotation such that the greater tuberosity of the humerus butts up to the scapula.
Shoulder impingement causes
Shoulder impingement can be caused by many factors, including
- quality of the soft tissues
- age
- flexibility
- anatomical variations
- joint mechanics
- posture.
The typical patient with subacromial impingement syndrome is over 40-years-old and reports pain without any known trauma. These patients may recall a shoulder injury following a repetitive movements, such as gardening and practicing tennis swings.
A “painful arc” is generally present when elevating their arm between 70 and 120 degrees, and pain can prevent them from lying on their side.
Rotator cuff pathology can be implicated in primary or secondary impingement. Swelling of the rotator cuff tendons may cause narrowing of the subacromial space in primary impingement.
The rotator cuff can be implicated in secondary impingement if weakness interrupts the ability of the muscles to depress the humeral head during arm elevation to steer clear of the acromion.
If the scapula does not upwardly rotate, posteriorly tilt, and externally rotate as a result of nerve entrapment, weakness, pain, or another cause, the scapula may not move out of the way of the humeral head during arm elevation.
[Read: Do I Need to Learn How to Fix Rounded Shoulders?]
Diagnosis of shoulder impingement
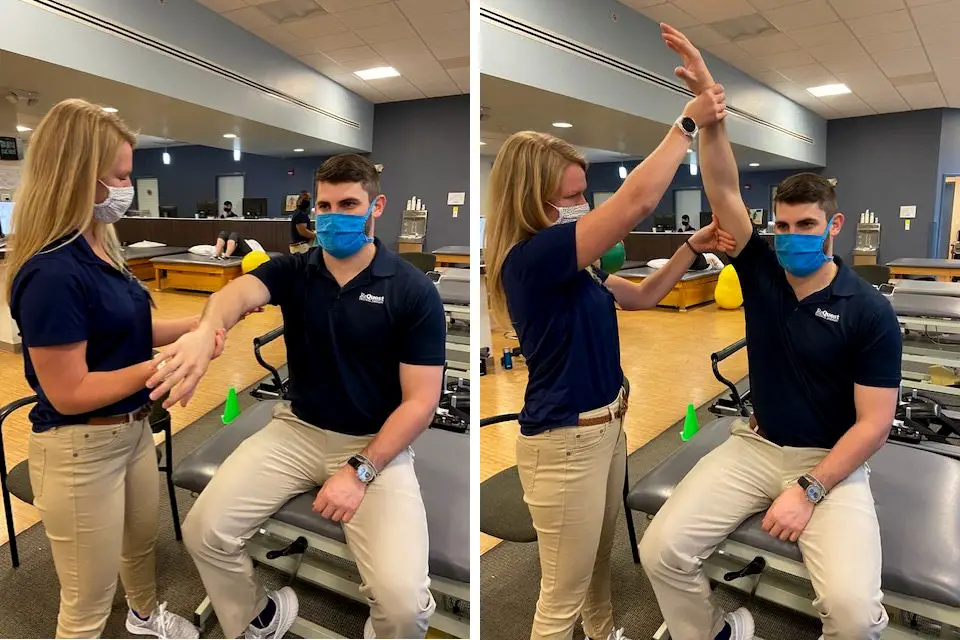
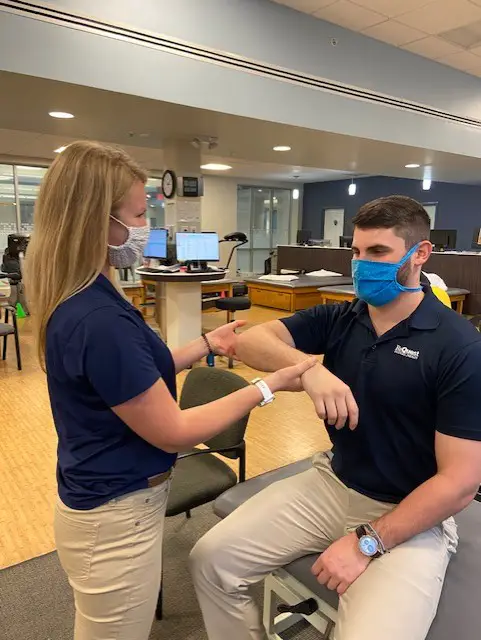
In a Neer test, the patient flexes the shoulder while the therapist apply pressure against the arm to see if there is pain. Photo: Penny Goldberg
Being diagnosed with shoulder impingement doesn’t always provide the clarity patients are looking for. This can be a “catch-all’ diagnosis that fails to implicate a specific structure which is sometimes frustrating for patients.
In my professional experience, this frustration can be mitigated by patient education. Informing patients about the complexities of shoulder anatomy and biomechanics is often useful to understand why their pain may not stem from a single structure.
As with all other musculoskeletal conditions, the crux of the diagnosis of impingement is a thorough history and physical examination. Patients may present with posterior shoulder stiffness or instability.
Special attention should be paid to the scapulohumeral rhythm to identify scapular dyskinesia, or abnormal movement. Hypermobility or instability of the glenohumeral joint should also be noted.
The most widely used shoulder impingement tests are the Neer, Jobe, and Hawkins-Kennedy tests. All of these tests are useful for concluding impingement is present but none are particularly good at isolating what structure is being impinged.
Pain with both the Jobe and Hawkins tests is indicative of subacromial impingement only; if internal impingement is present the tests will be negative.
The Neer test can identify the presence of subacromial or internal impingement depending on the location of the pain; anterior pain indicates subacromial impingement while posterior pain indicates internal impingement.
The Jobe test, often called the “empty can” test, can be paired with the “full-can” test to determine rotator cuff involvement.
If the patient experiences pain in both test positions, rotator cuff pathology is present and likely contributing to impingement. If pain is only present in the empty can position, the test is positive for impingement.
If pain is only present in the full can position, the test is positive for rotator cuff pathology. Taken together, if both are positive the impingement is likely caused by rotator cuff pathology.
Scapular dyskinesia is a catch all term for aberrant movement at the scapula. Newer special tests, such as the scapular assistance test, can help differentiate patients with pain caused by scapular dysfunction from those with other causes of impingement.
It may be clinically useful to use this test to rule out scapular dyskinesia as a source of pain.
On examination, a scapula that rests in more upward rotation is likely to be the result of a rotator cuff injury while a scapular that rests in downward rotation is likely to be the cause of dysfunction. In either case, physical therapy can help.
Although most patients with impingement don’t need imaging, it can provide insight into the problem. Radiographs are used to examine the shoulder, like measuring the acromiohumeral distance.
In most adults, this distance is 10 millimeters in men and 9.5 millimeters in women. Decreased acromiohumeral distance with no other specific anomaly visualized on imaging is indicative of rotator cuff pathology.
Although most injuries make activities of daily living challenging, the hardships associated with shoulder pain may be the worst. You need a combination of flexion, abduction and external rotation is necessary to reach overhead to style your hair, put on and take off your shirt, and take objects from high shelves or cabinets.
Extension, adduction, and internal rotation combine to allow reaching behind the back to fasten a bra, tuck in a shirt, or remove a wallet from a back pocket.
The research agrees with common sense when it comes to shoulder pain and disability. A 2009 cross-sectional study by Lentz and colleagues investigated the relationship of pain, physical impairments, and pain-related fear to function.
Range of motion measurements and outcome measures were collected on 142 patients with shoulder-related diagnoses. They reported range of motion and pain were correlated with higher levels of disability.
More recently, Anwer et al. investigated the relationship between pain, motion, and disability in patients with shoulder pathology. Sixty-four patients with a variety of diagnoses reported pain scores, functional ability, and range of motion measurements. In this cohort, flexion, abduction, and rotation range of motion were most associated with pain and disability.
Similar conditions to shoulder impingement
The differential diagnosis of shoulder impingement is complicated in that there are several underlying pathologies that may be related to impingement.
Some of the pathologies that need to be ruled out:
- frozen shoulders
- rotator cuff tears/tendinopathy
- scapular dyskinesia
- instability, biceps tendonitis
- labral tears
The signs and symptoms of most shoulder conditions are quite similar. Just to muddy things up a little more, pain may be caused by more than one structure or pathology at a time.
Patients with shoulder conditions may report the following regardless of diagnosis:
- Pain with overhead motion
- Pain when reaching out to the side
- Inability to lie or sleep on the involved side
- Tenderness at the front of the shoulder or mid-humeral region
- Aching at night
- Pain when reaching behind the back
- Weakness or stiffness of the involved side
Shoulder impingement treatments
When it comes to treatment, there’s strong evidence and anecdotal support for delaying surgery in favor of conservative management. Despite a lack research support, subacromial decompression (acromioplasty) surgery remains the most common arthroscopic procedure at the shoulder.
A period of three to six months of conservative management should be employed before you even consider surgery. The patient should be educated on activity modification that includes avoiding overhead movement, heavy mechanical loading, and repetitive motion.
A 2017 systematic review and meta-analysis in the British Journal of Sports Medicine concluded that exercise should be used in the treatment of this condition and that non-steroidal anti-inflammatories and corticosteroids were better than placebo for controlling pain.
Shoulder impingement exercises
Exercise selection for patients with shoulder impingement typically involves targeting the rotator cuff and scapular stabilizers. Choosing exercises that strengthen the posterior muscles and decrease rounded shoulders.
Bilateral external rotation
– Sit or stand with a tall posture and your shoulder blades set down and back (like you’re putting them in your back pockets).
– Bend your elbows to 90 degrees and pinned to your ribs.
– Hold a resistance band, dumbbell, soup can, or similar objects for resistance with your palms facing up.
– Pull your hands apart (thumbs go in opposite directions).
– Pretend like your hands are full of soup that you don’t want to spill. They should stay parallel to the ground through the full available range of motion and then come back together in the center of your body.
T exercise
– Use a counter, table, or back of the couch—something that can safely support your body weight.
– Hinge forward at your hips and support yourself on the forearm of your non-involved shoulder. The exercise starts with your involved side hanging straight down so that your fingers are pointing toward the floor and your palm is facing your midline.
– Set your shoulder blade down and back, and then raise your arm up until it is parallel to the floor. Your arm should come straight up so that if both arms were in this position you would look like the letter “T.” A common error in this exercise is to let the bigger, stronger muscles take over and raise your arm so that your hand ends up close to your hip.
– Your hand should be in-line with your shoulder in the finish position.
Prone W
– Lie on your stomach with your arms comfortably bent by your sides and your hands in-line with your ears.
– With your shoulder blades down and back, raise your arms off the floor until they are even with your body. From a birds-eye view, it should look like you are making the letter “W” with your arms and head.
Reverse kettlebell carry
– Hold a kettlebell or dumbbell over your head with your arm out straight. Your palm should face forward as if you are a waiter carrying a high tray.
– Engage your abdominal muscles and hold the weight steady while you walk for about 30 seconds. If you have to arch your back to hold the weight up, it’s too heavy.
Several studies have examined exercise intervention. A 2017 systematic review and meta-analysis investigated the use of specific vs. general exercise in the treatment of shoulder impingement syndrome.
Six randomized controlled trials were included in the review, and all the included studies used resistive exercises targeting proprioception, rotator cuff and/or scapular muscle strength, or stretching. The results suggest there is no evidential support for the use of specific vs. general exercises for targeting pain, function, range of motion, or strength.
Although exercise can treat of shoulder pathology, the type and amount of exercise have not yet been established.
Heron et al. wanted to find out what type of progressive loading exercises was most effective. A panel of experienced therapists chose three loading strategies after an extensive literature review:
- minimally loaded range of motion exercises
- open kinetic chain loading
- closed kinetic chain loading
All three groups had reduced pain and improve function, but no group was better than another. This may suggest that simply doing something to load the rotator cuff is the most important guideline to follow.
Shoulder impingement and massage therapy
The length-tension relationship of muscles is of utmost importance at the shoulder joint. This is one of the reasons we emphasize postural awareness in patients with shoulder pathology. The scapula alone has 17 muscular attachments which should make it easy to understand why proper positioning is critical to healthy shoulder function. A primary focus of tissue work should be ensuring the scapula is able to freely move throughout full shoulder range of motion.
One of the easiest ways to examine muscle length in the shoulder, and thus direct your treatment, is back-to-wall scaption. The patient stands with their feet six to eight inches from the wall and the low back pressed into the wall. They are instructed to raise their arms overhead until they reach the wall behind them or their low back can no longer stay pressed into the wall.

Photo: Penny Goldberg
They may also demonstrate forward head posture near the end range of available motion. If they’re unable to reach the wall, this indicates tightness in the rhomboids, pectorals, or latissimus dorsi muscles.
This position can be used for post-treatment assessment to determine the effectiveness of the intervention. You may also suggest moving in and out of this position repeatedly as a supportive exercise.
Patients with shoulder impingement tend to have tight external rotators (limited internal rotation motion). They can benefit from bodywork that addresses the rotator cuff muscles.
When working in the armpit to target subscapularis, it’s important to educate the patient that discomfort may be normal and that they should communicate to you anything that is intolerable.

Penny Goldberg, DPT, ATC
Penny Goldberg, DPT, ATC earned her doctorate in Physical Therapy from the University of Saint Augustine and completed a credentialed sports residency at the University of Florida. She is a Board Certified Clinical Specialist in Sports Physical Therapy.
Penny holds a B.S. in Kinesiology and a M.A. in Physical Education from San Diego State University. She has served as an Athletic Trainer at USD, CSUN, and Butler University.
She has presented on Kinesiophobia and differential diagnosis in complicated cases. Penny has published on returning to sports after ACL reconstruction and fear of movement and re-injury.
Outside of the clinic, Penny enjoys traveling, good cooking with great wine, concerts, working out and playing with her dogs.