Many patients tell me, “I noticed my right shoulder pain a few weeks ago but didn’t think much of it. Now, I have right arm pain when I sleep on my side, tuck in my shirt, or reach out in front of my body. Help!”
Some people can shrug off shoulder pain until it becomes a huge deal. Most of us don’t realize how often we use our arms everyday! They help us reach, carry, lift, dress, cook, eat, drink, type, write, use your computer mouse, and just about everything else you can think of.
I recently met a patient with left shoulder pain that started after a vacation in Mexico. During his trip, he jumped onto an inflatable float to send his kids flying in the air and then landed on his left side.

During his trip, my patient jumped onto an inflatable float to send his kids flying in the air and then landed on his left side.
He felt immediate left arm pain, especially when raising it out to the side, but it shrugged it off. But the pain worsened over the next three months before he came to see me. (Photo by Nick Ng.)
He felt immediate left arm pain, especially when raising it out to the side. The next morning he had a little bit of pain and stiffness but not so much that he couldn’t go on with his life. By the time he got to me three months later, he recalled occasional episodes of mild pain since the injury but in the clinic he was stiff, tight, and very painful.
As I listened to him, I thought it was either a torn glenoid labrum or a torn rotator cuff. He described deep aching pain, difficulty sleeping on his left side, feelings of instability, and occasional clicking and popping.
I planned to rely heavily on my special tests to make my diagnosis until I asked him to move his arm for me. Unlike some of our other body parts, several shoulder diagnoses can present with similar symptoms.
After watching him struggle to raise his arm above shoulder height or reach behind his body, I knew I had to also consider a frozen shoulder (officially: adhesive capsulitis).
Having pain when sleeping on the affected side, raising your arm out to the side, and reaching behind your back are the symptoms I hear most often in the clinic from patients with shoulder pain.
These symptoms can also come from a rotator cuff tear, glenoid labrum tear, impingement, or a strain.
To complicate things even more, shoulder pain can come from other joints or not be muscle-related in nature.
Cervical disc herniations, systemic illness (Kehr’s sign refers to left shoulder pain caused by a ruptured spleen!), or even stress can also cause arm or shoulder pain.
While special tests can be helpful, they can also be inconclusive or require positions the patient can’t get into because of pain or other symptoms.
In these situations, imaging can be helpful but it’s often expensive and may delay treatment while waiting for results. And more often than not, insurance companies require physicians to have patients try physical therapy before ordering advanced imaging.
Finding the right fit for the pieces of the shoulder pain puzzle can be difficult. Being willing to try a variety of treatments can be the first steps to putting it all together and reaching the correct diagnosis.
Shoulder anatomy
Shoulder anatomy is complex at best. From a bony standpoint, the glenohumeral joint (GH) doesn’t offer much stability and thus, relies heavily on thick, broad ligaments and muscles to keep everything in place.
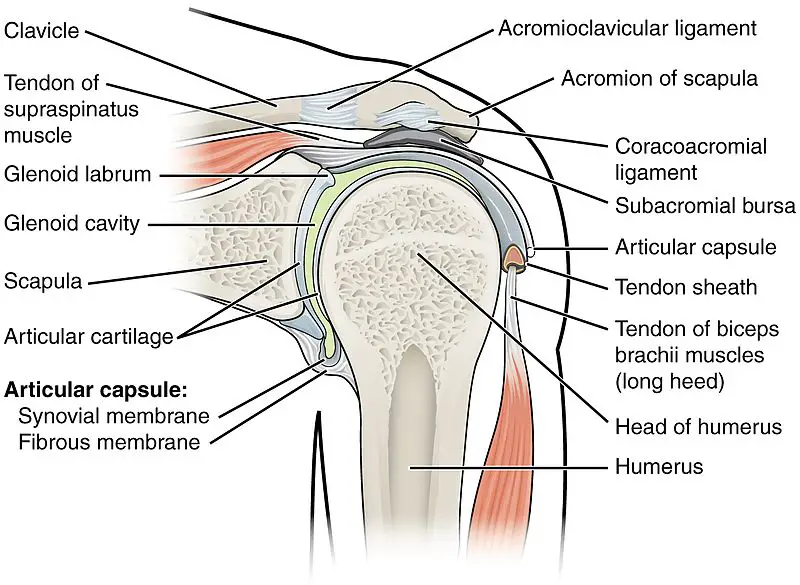
(Illustration by OpenStax College, Anatomy & Physiology, Connexions Web site. http://cnx.org/content/col11496/1.6/, distributed under the Creative Commons Attribution 3.0 Unported license.)
Often, this joint is described as a golf ball on a tee when it comes to visualizing the relationship between the humerus (arm bone) and the glenoid fossa of the scapula (shoulder blade).
The glenoid labrum works to create some stability by deepening the tee portion of the joint. Along with the labrum and glenohumeral ligaments, there are 17 different muscles attached to the scapula—a bone that’s hardly considered important by most laypeople.
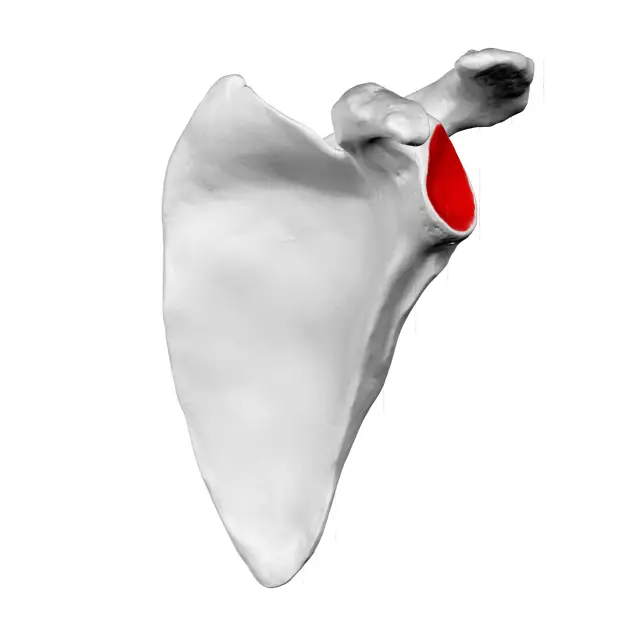
(Illustration by Polygon data is from BodyParts3D, distributed under the Creative Commons Attribution-Share Alike 2.1 Japan license.)
If you’ve been seeing a physical therapist for shoulder pain, you’re likely familiar with a cue similar to “start with your shoulder blades down and back.”
This scapular “set” position is important to shoulder movement because it allows the muscles to work from their optimal length-tension relationship.
When you work long hours on a computer or spend a lot of time driving, your muscles can become lengthened from poor postural awareness. As such, stretching the front of the shoulder and strengthening the back of the shoulder is often a critical element of shoulder rehab.
Timing is also important for healthy shoulders, which is called a scapulohumeral rhythm. The scapula creates a “roof” over the top of the humerus (via the acromion process), which requires these bones to work together when raising your arm above shoulder height. When they’re working well together, the subacromial space is maintained during motion.
Generally, the scapulohumeral rhythm is described as two degrees of humeral motion for every one degree of scapular motion or a 2:1 ratio, but this can vary widely among people.
If the timing is off, the humerus can get jammed up into the subacromial space and create shoulder pain.
The rotator cuff is another critical part of scapulohumeral rhythm. Most of us think of the rotator cuff as a group of muscles that are used to throw a baseball or football, but it also plays a major role in keeping the humerus seated on the glenoid. From the original analogy, these muscles keep the golf ball centered on the tee.
When the rotator cuff is weak or painful, it can lose the ability to maintain this position which allows the humerus to ride up into the subacromial space.
Decreasing this space can cause injury or irritation to the other structures that live there, like the supraspinatus, biceps tendon, and subacromial bursa.
Types of shoulder pain
Highlight the following types of shoulder pain. What should the patients know about them if they were to just scan each section for a few seconds?
Shoulder impingement syndrome
Shoulder impingement syndrome is a catch-all term used to describe rotator-cuff-related shoulder pain. This describes all of the conditions that cause a decrease of the subacromial space which causes the structures housed there to be pinched or impinged.
Frozen shoulder
Frozen shoulder, known officially as “adhesive capsulitis” is a condition where there’s a high pain level and limited range of motion. Your shoulder can “freeze” as a result of an injury or for no reason at all.
Rotator cuff tear
Rotator cuff tears come in all shapes and sizes. The effect they have on shoulder pain and function is well correlated to the size of the tear (bigger tears mean more pain and dysfunction).
Small to moderate tears can usually be managed with conservative treatment while larger tears may need to be surgically repaired to regain function.
Bankart’s lesion
A Bankart’s lesion is a tear of the glenoid labrum that’s typically caused by one or more shoulder dislocations. Bankart tears can be soft (labrum only) or bony (labrum tear or glenoid fracture) and may require surgery to restore shoulder stability.
Shoulder bursitis
Shoulder bursitis can result from overuse/irritation, systemic illness (diabetes, gout, rheumatoid arthritis), bacterial injection, or trauma due to an accident or fall.
There are five main bursa around the shoulder joint. Although any of them can develop bursitis, subacromial bursitis is the most common location.
Shoulder arthritis
Shoulder arthritis can occur in any of the joints that make up the shoulder girdle but is most often found in the GH and acromioclavicular (AC) joints.
To some extent, arthritis is part of the normal aging process; just like we get wrinkles in our skin, this is just “wrinkles” on the inside.
The effects of arthritis can’t be reversed but you can slow the process by giving your joint the best environment to function, such as preserving the remaining range of motion, flexibility, and strength.
What causes shoulder pain?
Shoulder pain can have a variety of causes, and it rarely has a single cause.
AMBRI
In younger shoulders (ages 10 to 30 years old), the primary cause is likely to be related to instability. Such instability can be categorized as AMBRI:
A = atraumatic
M = multidirectional
B = bilateral
R = rehab
I = inferior capsular shift/plication
You can probably see the symptoms of AMBRI with an MRI. In these cases, imaging will likely be trivial as there isn’t an injury to see. That said, an MRI can give you a peace of mind so you can commit to a conservative rehab program.
And so, physical therapy that focuses on strengthening, co-contraction, and coordination is generally the first line of treatment. A 2015 systematic review by Longo et al. analyzed the outcomes conservative and surgical treatment in patients with multidirectional instability.
The group found that less than 25% of patients failed exercise-base management and ultimately required surgical stabilization.
Stretching these patients is unlikely to be necessary or helpful. Surgery should be a last resort if the patient has failed several months of conservative rehabilitation.
TUBS
Shoulder pain that is classified as TUBS often has a distinct onset such as a sports injury or fall. TUBS stands for:
T = traumatic
U = unidirectional
B = Bankart (Hill-Sachs) lesion
S = surgery
These patients may report dislocation or subluxation and have an MRI that shows a Bankart lesion, Hill-Sachs fracture, or both.
Bankart lesions (injury to the anterior inferior labrum) are typically caused by a shoulder dislocation. At times, the back of the humeral head can have a secondary injury caused by the forceful contact with the scapula as it moves back into place when dislocated.
Overuse
The next most common diagnosis in younger shoulders is overuse. This age group is likely to do too much, too soon, and too often. In this context, overuse includes gross internal rotation deficit (GIRD) and scapular dyskinesis.
Overhead athletes who report shoulder and/or elbow pain may also have GIRD. They often describe workout regimens that involve throwing or pushing but the pain isn’t necessarily explainable by a single event.
Athletes with GIRD often show weakness in their scapular stabilizers and tight chest and back muscles. Imaging is unlikely to be helpful in making a diagnosis and usually only occurs if the patient has failed physical therapy.
Scapular dyskinesis
Scapular dyskinesis is a scary-sounding term for something that’s relatively common. It’s a catch-all term for dysfunctional movement of the shoulder blade that may be caused by weaknesses and tightness of the shoulder joint. Rotator cuff injury or nerve entrapment can also cause scapular dyskinesis.
In 30- to 50-year-old shoulders, the primary diagnosis is a rotator cuff tear (likely partial). These patients report painful overhead motion, pain when reaching behind their back, and difficulty sleeping on their painful side.
The pain has usually come on gradually and movement is painful while range of motion remains full. Rotator cuff strength in these patients may not be dramatically weak. Imaging may be helpful to rule out severe tears or to visualize the extent of tendonitis/tendinosis that may be present.
One complication of shoulder diagnosis in this age group is the secondary diagnoses that result from partial rotator cuff tears.
In patients where rotator cuff weakness is present, there may be encroachment on the subacromial space which results in shoulder impingement syndrome (SIS) or subacromial bursitis.
More recently, clinicians have moved away from these labels in favor of a more general term—rotator cuff-related shoulder pain or even non-specific rotator cuff-related shoulder pain.
There are two additional diagnoses that are frequently seen in 30- to 50-year-old patients: frozen shoulder and acromioclavicular joint (AC) arthritis.
The patient’s history will usually tell the story in AC joint arthritis; often a history of weight training with heavy overhead pressing movements or playing overhead sports will predate this shoulder pain.
Conversely, a frozen shoulder usually comes out of the blue. At times, it can occur after a shoulder surgery to address another issue or after an injury.
In people more than 50 years old, the primary diagnosis is usually a full-thickness rotator cuff tear. Similar to their younger counterparts, these patients have pain with overhead motion and internal rotation, pain at night, and referred pain to the middle of the upper arm or into their elbow.
This shoulder pain is also typically gradual in onset but the weakness may be dramatic before they seek treatment. Occasionally, full thickness rotator cuff tears are seen following trauma, such as a motor vehicle accident or a fall.
Clinicians may see changes in the way you move your shoulder, indicating that some muscles are substituting for others to help raise your arm overhead.
Shoulder pain treatments
Shoulder pain treatments can be quite variable. While exercise is (almost) always the best modality, it can be complemented by a host of other treatment options to address symptoms, such as pain or tightness.
Exercise
Research shows that exercises that strengthen the rotator cuff and scapular stabilizer muscles are the most common first-line approach for the treatment of shoulder pain.
An international team of researchers made a strong recommendation in a 2020 systematic review for including exercise in the treatment of shoulder pain.
While the authors found high- or moderate-level evidence that included exercise as a treatment, most of the studies didn’t describe the details of the program, so exercise selection, dosing, and intensity is less clear.

When the technique, dosage, and programming are done correctly, weightlifting can be part of the shoulder pain rehab. (Photo by Andres Aryton.)
For some conditions, exercises that address the muscles that help keep the scapula in the “down and back” position are typically given early in a patient’s plan of care.
Sometimes exercise is a way to get you moving when you stay in one position for too long. At times, the discomfort you feel can simply be your body telling you that it wants to move.
Surgery
There are several shoulder surgical options that depend on the location and extent of the injury.
Rotator cuff or glenoid labrum repairs are not all created equal. A larger tear in either structure will require a surgeon to fixate your shoulder to restore stability.
How long you stay immobilized and go through rehab depends on the complexity of the procedure that was performed.
A subacromial decompression (SAD) may be performed with another procedure or by itself. A SAD, also called a “Mumford Procedure,” involves shaving down the acromion process of the scapula to free up the subacromial space. This procedure can help patients with subacromial bursitis, biceps tendonitis, and rotator cuff injuries.
When the biceps tendon is irritated beyond repair, a tendon surgery called “biceps tenodesis” may be performed. Here, the surgeon moves the long head of the biceps tendon from the top of the glenoid process (where it’s flush with the labrum) to the middle of the humerus to decrease irritation from a torn labrum or decreased subacromial space.
Arthroplasty
There are two options for arthroplasty of the shoulder joint. The difference between the two procedures from a mechanical standpoint is that in the reverse total shoulder, the scapular prosthesis is the “ball” and the humeral side is the “socket.”
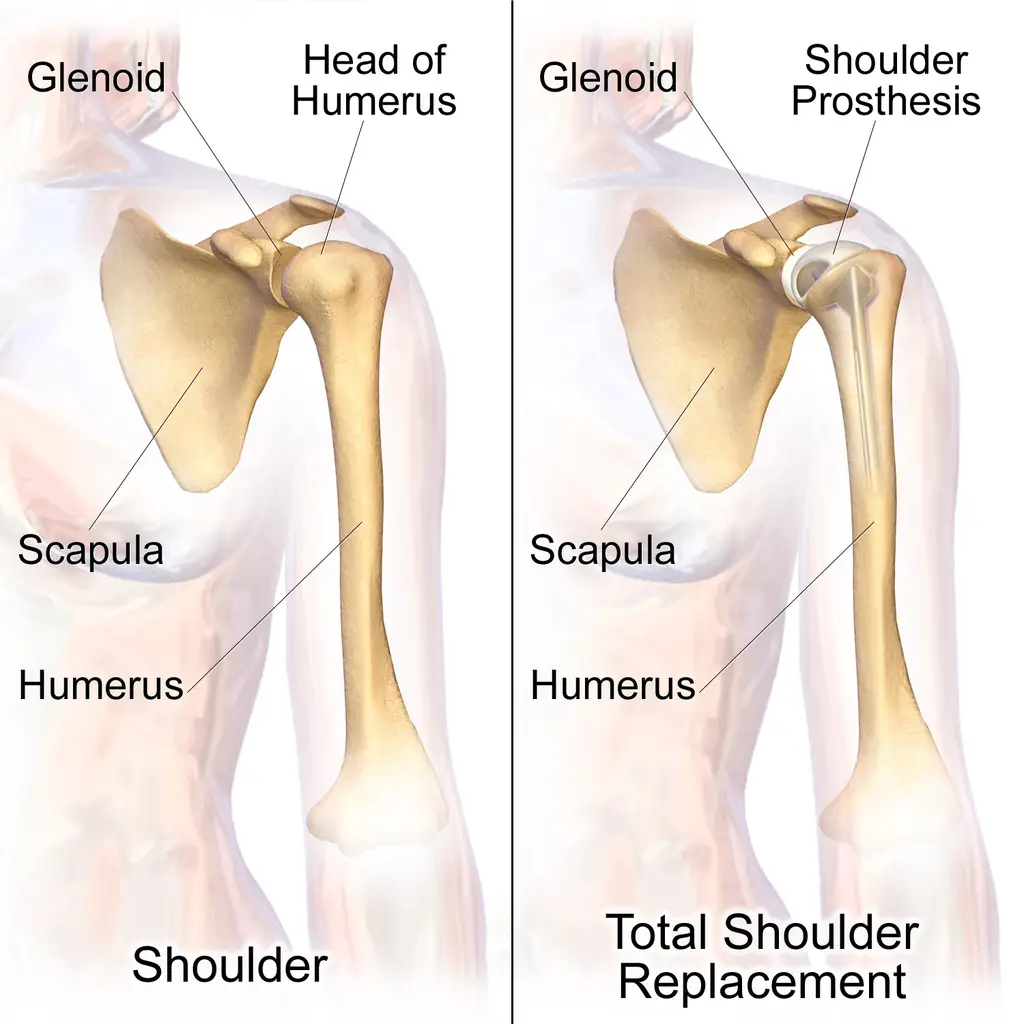
Normal shoulder vs. full shoulder arthroplasty. (Illustration by BruceBlaus, distributed under a Attribution-ShareAlike 4.0 International (CC BY-SA 4.0) license.)
Patients with a functioning rotator cuff can have a total shoulder arthroplasty. The reverse total shoulder arthroplasty is reserved for patients without a working rotator cuff.
Injections
Corticosteroid injections (CSI) are often used to calm the pain and inflammation you are feeling long enough to make rehab possible. They’re rarely meant to be a stand-alone treatment but rather seek to bridge the gap between pain and function.
It may take more than one injection to achieve pain relief, but most physicians will look for other options if CSI seems to provide less pain relief or wear off faster than they previously had.
Steuri et al. examined the effectiveness of conservative treatments for adults with shoulder impingement. Their systematic review and meta-analysis found evidence that CSI is better than active modalities for improving pain and function but these effects only lasted through the shortest follow-up period.
This is consistent with the idea that CSI works well as a stop-gap for pain so that you can carry out rehabilitation exercises.
Lidocaine injections may also be used to address the pain associated with frozen shoulders. If you have it, the rehab process can be downright miserable so this fast-acting, short-lasting medication may be used to make your treatment tolerable.
TENS
Transcutaneous electrical nerve stimulation (TENS) can be quite effective at relieving shoulder pain however the relief only lasts as long as the machine is attached.
By targeting the smaller, faster A-delta nerve fibers, TENS works as a counter-irritant to pain by sending a vibration signal to the brain ahead of the pain signal coming from your shoulder, which, in turn, provides pain relief.
This mechanism of action is akin to what happens when you hit your thumb with a hammer. If you shake your hand or run it under cold water, the vibration or temperature act as counter-irritants to the pain by signaling their sensation to the brain via the faster transmitting nerves.
In managing shoulder pain, TENS seems to have similar effects to CSI. Both CSI and TENS improve shoulder pain in patients with rotator cuff tendinopathy but neither persisted beyond the short-term.
Massage therapy
Massage therapy can be a useful adjunct to traditional shoulder rehab because it addresses both direct and indirect impairments of the shoulder pain.
Direct effects of shoulder pain that benefit from massage are tight pectoral, internal rotator, and external rotator muscles. Using massage to create overall relaxation can help your shoulder move through a larger range of motion with less pain.
Although massage therapy may provide temporary shoulder pain relief, it may help you further manage your symptoms as you heal. (Photo courtesy of Zack Miller.)
Also, shoulder pain can lead to neck pain because the neck muscles will work hard to help move a weak or painful shoulder. Including the neck muscles in massage therapy sessions can also help restore shoulder and arm function.
Researchers have found massage to be an effective treatment for decreasing pain and improving range of motion and function in patients with non-specific shoulder pain.
But there’s not much high-quality evidence but the smaller sample sizes and short follow-up periods show promising results. Massage therapy that targets the scapular muscles, performed in the end-range of motion positions, seems to be the most effective.
Chiropractic for shoulder pain
Chiropractic care for the shoulder may include treatment that focuses on the neck or rib cage if those regions are thought to be impacting your shoulder pain and function.
A chiropractor will also likely teach you a home exercise program to help relieve your shoulder discomfort and improve function.
There’s limited evidence to support chiropractic care for shoulder pain but this doesn’t necessarily mean it doesn’t work—only that there aren’t enough high-quality studies to draw meaningful conclusions.
A 2010 systematic review suggests manipulation is useful for short-term pain relief in patients with subacromial impingement. The review cites more than 25 case reports and case series that support the use of chiropractic care for managing shoulder pain, especially when different treatments are used.
KT tape and shoulder pain
To tape or not to tape—that is the question.
The answer is why not?
Kinesio Tape, the wildly popular fad that you may have seen on Olympians, CrossFitters, and grandmothers alike, has been claimed to lift the skin so that the underlying tissues are under less pressure.
The lift created by the tape improves the movement of lymphatic fluid. Decreasing the pressure on the tissues may also help reduce pain or discomfort.
But this is physiologically impossible, said exercise physiologist John Brewer, unless “there is a force in the opposite direction, such as pushing down on the skin.”
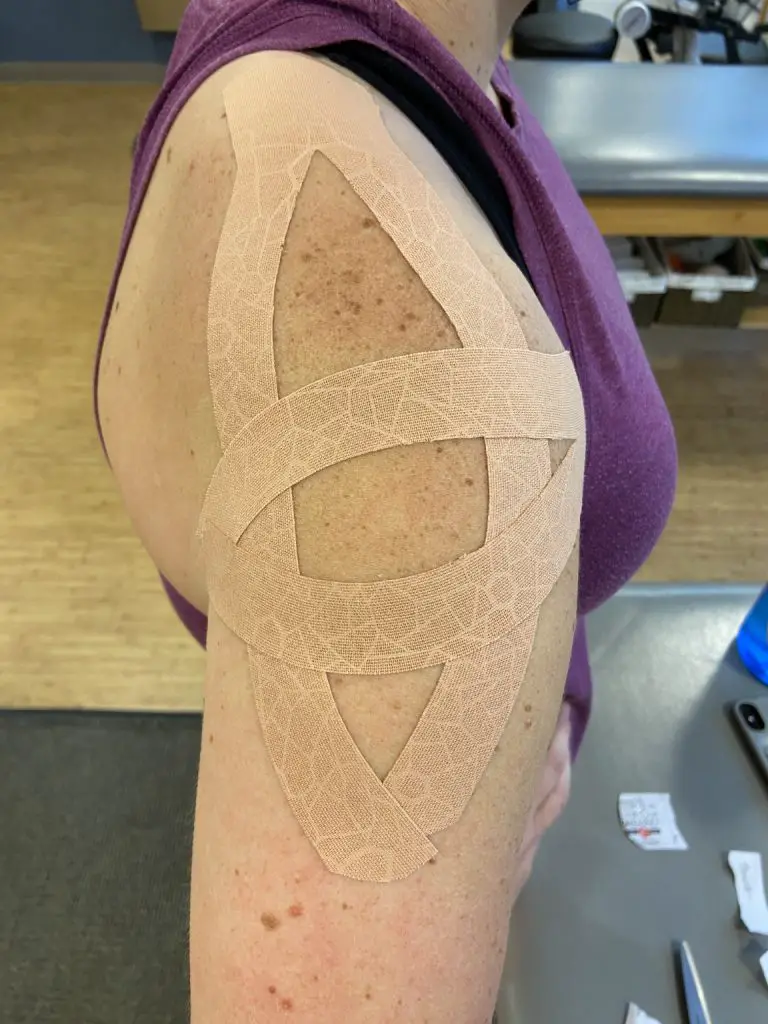
Kinesio taping or using any kind of athletic tape may provide short-term pain relief to help you complete your competition or practice. (Photo by Penny Goldberg.)
Most brands of kinesio tape also suggest that wearing the tape provides support to the working muscles so that the effects of overuse are delayed.
Videos on how to apply kinesio tape to the shoulder are a dime-a-dozen online despite most of the research lacking support for its use.
Systematic reviews and meta-analyses by Celik and colleagues, Ghozy et al., and Parreira et al. looked at more than 1,500 shoulders and all found Kinesio Tape was no more effective than any other treatment.
That said, there’s some weak support for the use of kinesio tape in those with rotator cuff tendonitis or impingement.
Patients who were taped for two consecutive three-day intervals immediately showed improvements in pain-free shoulder motion.
Although pain and disability were unchanged, kinesio tape may have value in providing a path to tolerating a larger range of motion during rehab without needing more invasive treatments.
Carpal tunnel and shoulder pain
Carpal tunnel syndrome is a common diagnosis that describes a condition where the nerves that travel through the carpal tunnel are irritated.
From a general anatomical standpoint, nerve pain does not travel toward the midline of your body. When a nerve is injured, the direct effects of the compression are thought to be found ‘downstream’ but this may not always be true.
In a study of 56 patients with carpal and cubital tunnel syndromes, Hagiwara et al., those who had shoulder pain, pain or tingling with compression of the medial nerve at the wrist, and Tinel’s sign along the ulnar nerve were included in the study.
In this group, six patients had more than 60% pain relief from a wrist splint alone, 23 patients had nerve blocks that relieved their symptoms and improved shoulder motion, while 27 needed surgery in the end.
Although these results aren’t overwhelming in either direction, more than 50% didn’t need surgery which is worth considering.
In carpal tunnel, you may experience indirect pain caused by activity changes that are used to fend off symptoms at the wrist or hand.
For example, if your wrist pain forces you to change the way you hold your phone, control your steering wheel, or what position you sleep in at night, you could develop a related case of shoulder pain. And so, treating only the shoulder won’t likely yield positive results.
COVID and shoulder pain
COVID-19 has impacted all of us in very obvious ways—shutdowns, supply chain issues, and social implications for starters.
For others, the effects of COVID-19 may include long-lasting physical disabilities.
Treatment for COVID-19 related pneumonia is treated with mechanical ventilation in the prone (face down) position to improve oxygenation. Patients can be placed in this position for days, weeks, and even months at a time.
Alvarez et al. examined shoulder pain in COVID-19 survivors after being on mechanical ventilation. In their group, 20 patients were evaluated by a physical therapist for pain, decreased motion, and decreased strength in their shoulder.
Eighteen of these patients underwent further diagnostic testing that showed the following diagnoses:
- median nerve damage
- carpal tunnel entrapment
- rotator cuff tendinosis/tendinopathy
- frozen shoulder
- AC arthritis.
All of these conditions were attributed to lying facedown.
Also, 1% to 65% of long COVID sufferers may experience shoulder pain. It can be localized to a specific region or widespread. Not enough is known about long COVID to predict how this pain progresses over time.
Psychosocial factors of chronic shoulder pain
It’s impossible to overstate how important the use of our arms and hands are to everyday life. Losing function in either or both can be life altering to say the least.
“In many cases, the upper extremity may even have the greatest tie into the psyche due to the relationship between the upper extremity and daily function,” said Dr. Debi Jones, a double-board certified physical therapist at the Hospital for Special Surgery in Westchester, New York.
She emphasized that fear of movement and expecting the worst case of pain episodes can lead to a “cycle of disuse” that will affect your strength, range of motion, and function.
“Your hands are what you use to touch, explore, and manipulate the world around you and are therefore intimately tied to your identity as a human,” Jones said.
Shoulder arthroplasty and race
Joint replacement as a treatment for severe arthritis is thought to be a common treatment when non-surgical options have been exhausted. Studies show these procedures may not be common to everyone.
Researchers found that even when Black and non-Black patients have similar clinical, demographic, and socioeconomic characteristics, Black patients are less likely to access care services.
Among the 256,000-plus patients undergoing arthroplasty from 2005 to 2011, less than 4% self-identified as Black.
This appears to be a problem that begins long before the need for surgery arises. When comparing the care provided to Black and White patients, surgeons tend to spend less time educating Black patients about biomedical concepts and on general relationship building.
As a result, these patients are less likely to know about arthroplasty as a treatment option and are unlikely to know anyone who has had the procedure.
Shoulder pain, race, and gender.
Gender, race, and age of a patient all seem to impact pain management decisions at the provider level. In a 2013 study from the University of Florida, researchers used virtual patients to study the role of these demographic factors on 193 healthcare professionals’ pain ratings.
The nurses and physicians in the project assessed virtual patients who were male and African American to have more intense pain and were thus more willing to prescribe opioid medications to them.
Of the two healthcare professions, nurses were more likely to assign higher pain ratings and were more willing to prescribe opioid drugs than their physician counterparts.
The biases revealed in this study suggest that patient demographic cues may influence pain management decisions.
In a 2019 scoping review by Meints et al., the researchers highlighted the complex psychosocial mechanisms that may play a role in racial and ethnic disparities in the treatment of pain.
Some of the factors of poor treatment include:
- language barriers
- access to interpreters
- health literacy
- culturally different communication styles
Dr. Samantha Meints, who is a pain psychologist at Brigham & Women’s Hospital in Chestnut Hill, Mass., and led the study, said that the burden of costs and chronic pain is more prevanlent among those in the BIPOC communities in the U.S.
“In this review, we not only wanted to highlight some of the mechanisms driving pain disparities but also identify future research targets and possible solutions for reducing BIPOC disparities in pain,” Meints said. “I have two broad programs of research. In the first, I hope to better understand and ameliorate disparities in the experience and treatment of pain. In the second, I am working to develop and implement nonpharmacologic treatments for the prevention and treatment of chronic pain. Together, I hope that we can decrease the rates of chronic pain and improve quality of life.
In the future, they suggest efforts to address provider- and system-level factors, such as using communication styles that cater to the individual patient and community support groups.
“To a patient trying to navigate a really difficult healthcare system, I encourage patience while also being persistent and taking an active role. Data has shown that chronic pain is not easily treated and that, often, medications, surgeries, and injections will not ‘cure’ their pain,” Meints suggested. “Instead, patients have to learn self-management techniques to live with pain but in a way that still affords them a quality of life.
“For example, patients may need to engage in physical therapy to gain strength and stamina. Many patients get frustrated that this does not reduce their pain. However, if they understand that the goal is to be more functional with the same or less pain, perhaps they would be more inclined to engage in this kind of treatment. The same is true for pain psychology, which is the work I do. I do not have a magic wand but I can help patients gain knowledge and skills to better cope with pain and get back to doing the things they love.”
Who is the “best” physical therapist and massage therapist near me for shoulder pain?
Finding the “best” physical therapist and massage therapist near you can be challenging. If you know someone who has been through shoulder pain, asking them for a recommendation can go a long way.
If you don’t know someone, reading Google reviews, patient testimonials, and therapist biographies can paint a pretty good picture, too.
Most private-practice physical therapists also offer free screenings. This can be a great way to get a few minutes of Facetime with a clinician.
However, they’re unlikely to give you a detailed plan of care during this meeting but most will explain their general approach and explain how they think they can help you.
The physician who is writing the referral to physical or massage therapy may also suggest a clinician they know, like, and trust.

Penny Goldberg, DPT, ATC
Penny Goldberg, DPT, ATC earned her doctorate in Physical Therapy from the University of Saint Augustine and completed a credentialed sports residency at the University of Florida. She is a Board Certified Clinical Specialist in Sports Physical Therapy.
Penny holds a B.S. in Kinesiology and a M.A. in Physical Education from San Diego State University. She has served as an Athletic Trainer at USD, CSUN, and Butler University.
She has presented on Kinesiophobia and differential diagnosis in complicated cases. Penny has published on returning to sports after ACL reconstruction and fear of movement and re-injury.
Outside of the clinic, Penny enjoys traveling, good cooking with great wine, concerts, working out and playing with her dogs.