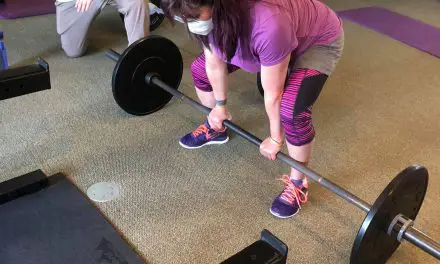Since massage therapy can help alleviate pain for many types of chronic pain conditions, it’s likely that it can also help your rheumatoid arthritic symptoms.
Before answering what massage can do, let’s see what rheumatoid arthritis is from a scientific and two patients’ perspectives.
What is rheumatoid arthritis?
Rheumatoid arthritis — or RA — is an autoimmune disorder that lasts a lifetime. It typically affects your joints, like fingers, shoulders, and knees, but it may affect your eyes, lungs, blood vessels, skin, and heart.
Whether arthritis is a disease or a disorder is debatable. Arthritis.org states that the term is an “informal way of referring to joint pain or joint disease.” But some scientists say that it’s a “chronic inflammatory autoimmune disease” that is influenced by genetic, epigenetic, and environmental factors.
Rheumatoid arthritis is categorized as a type of undifferentiated connective tissue disease. This is a broad term that describes the disease having signs and symptoms of one or more connective tissue diseases, but it doesn’t have specific traits of any one disease. This makes diagnosis and treatments tricky and risky.
Because it’s an autoimmune disorder like scleroderma, EDS, and lupus (SLE), your immune cells attack your healthy connective tissues in rheumatoid arthritis.
While there’s no cure for RA, there are treatments that can manage your symptoms to stop or slow its progression.
What causes rheumatoid arthritis?
While no one really knows what causes rheumatoid arthritis, there are some clues in research that show some factors can increase the likelihood of getting RA.
Basically, your immune cells get into your joints and their connective tissues from your blood vessels. They “attack” your tissues, causing inflammation and swelling of your joints, which can be painful and quite warm to the touch.
One type of antibody called ACPA (anti-citrullinated protein antibodies) has been found to be a highly predictive indicator to having rheumatoid arthritis.
Genetics
A change in one or a few genes in some types of proteins that are needed in cell communication (cytokines) have been linked to developing RA. Whether this change occurs in one gene (“SNP”) or to a gene expression without changing the DNA sequence (“methylation”), both have been shown to increase the risk of getting RA.
Environmental
Smoking has been shown repeatedly in research to be a significant factor in developing rheumatoid arthritis, even among children. In fact, a recent longitudinal study of more than 90,000 women — all nurses — between the ages of 35 to 52, were asked a questionnaire about their condition every two years from 1989 to 2017.
While the researchers found “no significant” association between RA risk with maternal smoking during pregnancy or living with smokers after age 18, they found that persistent childhood exposure to cigarette smoking from parents is a significant factor in developing rheumatoid arthritis.
Other environmental factors include:
Organic and inorganic dust: A large Swedish study of more than 12,500 cases of rheumatoid arthritis with matching 129,000+ controls found that exposure to textile and animal dust “are associated with increased risk of RA” provided that there is further evidence that the airborne exposures are a major cause of RA.
Damage and/or inflammation of the various lung tissues due to asthma is tied to cigarette smoke exposure and air pollutants.
Viral infections of the lungs: A South Korean study of more than 24,000 people with rheumatoid arthritis found that those who were exposed to the coronavirus (not COVID-19), parainfluenza, and metapneumovirus had increased the flare ups and other symptoms of RA. But the researchers said that this is by no means proof of a cause-and-effect relationship.
Overweightness and obesity has been shown to increase certain gene expressions that contribute to joint inflammation.
Overall, it appears that rheumatoid arthritis isn’t caused by any singular factor. Like our pain experience, a combination of several or many factors increase your risk of getting RA.
What are the first signs of rheumatoid arthritis?

“I expected to go back to my job, but whenever I tried to get healthier like exercise or trying to work, I noticed those symptoms were still there but they were way worse.” Photo: Eileen Davidson
Early signs of rheumatoid arthritis include:
- Pain, stiffness, and/or achiness in more than one joint
- Swelling and tenderness in more than one joint
- Such symptoms almost always occur symmetrically in your body
- Fever
- Extreme fatigue
- Weight loss
- Weakness
Sometimes the symptoms can be mistaken for other conditions. For Eileen Davidson, who is a Canadian advocate for rheumatoid arthritis patients (Arthritis Research Canada), she had spent most of her twenties thinking that her chronic joint pain in her hands were from carpal tunnel syndrome.
Before she had the early symptoms of rheumatoid arthritis, Davidson was working as an esthetician in Vancouver, B.C., in her early twenties.
After many years of working in pedicures, massages, and facials, her hands, shoulders, neck, and feet hurt a lot. It wasn’t the typical aches and pains that go away after rest; her pain stubbornly persisted and sometimes flared up.
“From age 24 to 26, my job was getting more difficult and the pain was increasing,” she said. “I didn’t really understand why, and I was also getting sick a lot. I’m catching colds and flus, and it took me a long time to get rid of them.”
When was pregnant with her son at age 26, Davidson, who still didn’t know she had rheumatoid arthritis yet, struggled with the same symptoms.
“During my pregnancy, I didn’t feel any better,” she said. “A lot of women say they’d feel better during pregnancy, but I definitely didn’t. After my pregnancy, I expected a lot of the symptoms to go away — like my swollen feet and hands and depression.
“I expected to go back to my job, but whenever I tried to get healthier like exercise or trying to work, I noticed those symptoms were still there but they were way worse.”
Davidson had spent the next three years working as an esthetician despite having severe pain and fatigue until she was diagnosed with rheumatoid arthritis at age 29.
Osteoarthritis vs. rheumatoid arthritis: what’s the difference?
Sometimes the symptoms of rheumatoid arthritis can be mistaken for osteoarthritis. But here are some features that you can distinguish between them.
Osteoarthritis is usually caused by physical injury, usually from “wear and tear.” Damage of articular cartilage, which is the film of tissues that covers the ends of two bones of a joint where they form a joint.
Rheumatoid arthritis, as mentioned earlier, is an autoimmune disease (or disorder) where your immune cells damage healthy tissues, mostly in your joints.
Other differences include:
- Joint pain and inflammation are usually one-sided in osteoarthritis while they often occur symmetrically.
- People about age 60 and older tend to develop osteoarthritis, while rheumatoid arthritis can happen at any age, even among children and young adults.
- Your joints usually get less stiff and painful the more you move if you have RA, but not so with osteoarthritis.
- Different biomarkers: genetic tests among patients with either osteoarthritis or RA find that each disease exhibits different biomarkers — substances in your body that physicians and lab techs use to identify what condition(s) you have.
What are the 4 stages of rheumatoid arthritis?
Some research indicate that rheumatoid arthritis undergoes four stages of progression. It can take many years to reach the final stage, and everyone experiences different symptoms and speed of the progression. A group of Australian researchers highlighted the stages as:
Triggering stage: stage 1 of RA is where your immune cells attack your joints’ connective tissues, triggered by genetic and environmental factors. Your bone tissues aren’t affected yet.
Early symptoms include joint stiffness, particularly in the morning, and mild swelling of your joints. This stage is often too early for clinicians to determine whether you actually have RA or something else; thus, this is called “unclassified arthritis.” This term may be carried over to the next stage.
Maturation stage: At stage 2, your body makes more antibodies from your bone marrow and lymph tissues, which causes swelling and pain in your joints. ACPA levels are quite high enough to be detected in blood tests.
At this stage, the swelling, rheumatoid nodules, and other symptoms will likely come and go for several years before RA becomes onset in your joints. Cartilages and other connective tissues are gradually degraded.
Targeting stage: The symptoms at stage 3 are now more visible in the hands, fingers, and other joints. Symptoms of the finger and foot joints are often bent and crooked with limited movement. Sometimes the nerves in the joints are pinches, which may cause pain.
The bursae and tendon sheaths are degrading to the point where the joints will be bone-on-bone contact.
On a cellular level, research has shown that there is a huge amount of immune cells (macrophages) in synovial membranes, and an imbalance of two different types of such cells — pro-inflammatory vs. anti-inflammatory — are significantly higher among RA patients than non-RA people.
Among RA patients, the ratio of anti-inflammatory macrophages are lower than pro-inflammatory ones. This imbalance causes the rate of bone degradation to be much higher than the rate of bone formation.
Fulminant stage: The final stage is where you can no longer move your joints much or at all. As the term “fulminant” implies, the joints have fused together and rheumatoid arthritis is at full onset. There is heavy damage to the cartilage and bone.
Also at this stage, there is an increased risk of getting cardiovascular disease due to systemic inflammation.
Other complications include increased risks of :
- Reduced cognitive function
- Fatigue
- Lung tissue inflammation
- Fibrotic disease
- Sarcopenia
- Sjogren’s syndrome
- Cancer
Who is more likely to get rheumatoid arthritis?
About 0.5% of the world’s population suffer from rheumatoid arthritis, with people who live in urban areas have higher prevalence of the disease than those in rural areas.
In addition to genetics, certain viral infections, air pollutants, and obesity mentioned earlier, other factors that increase the likelihood of getting RA include:
Gender: Women are about three to four times more likely than men to get RA, but data suggests that it mostly pertains to women age 50 and under. At around age 60 for both genders, the ratio for women and men decreases to 2:1.
One reason why women are more likely to develop rheumatoid arthritis is because of higher levels of a certain form of estrogen hormone.
Age: While rheumatoid arthritis is often assumed to occur in older people, it can happen at any age.
Ethnicity: A 2017 review of nearly 8,800 Americans found that being full or partial Hispanic have lower risk of getting rheumatoid arthritis. The authors wrote that it could be a statistical issue since the majority of the sample (40.7%) are whites while the remaining samples are nearly 20% are Blacks (non-Hispanic), Mexican American and other Hispanics, and other ethnicities.
Socioeconomics: The same review also found that “living in poverty and covered by health insurance were also positively associated with RA,” but there is no cause-and-effect relationship established.
Other factors that can increase the risk of getting RA include having diabetes or osteoarthritis. Getting enough sleep regularly and a lack of sufficient vitamin A intake were associated with a lower risk of RA. Again, the researchers only found associations, not causation.
Complications of rheumatoid arthritis
People with rheumatoid arthritis tend to have a shortened lifespan of three to ten years because it comes with various complications that are different for everyone due to its systematic nature.
These complications include:
Lung disease: First identified in 1948 to be associated with RA, lung disease can come in various types and symptoms, including pleura disease, rheumatoid lung nodules, and pulmonary hypertension.
Cardiovascular disease (CVD): Various types of CVD include heart failure, arrhythmia, pericarditis, myocarditis, atherosclerosis, and valve disease. People with RA have a mortality rate 1.5 to 3 times higher than the general population.
Paresthesia: Whether you feel a persistent pricking or burning sensation in your joints, symptoms of paresthesia include peripheral nerve inflammation and nerve impingement. It can also affect your central nervous system, which may cause cervical myelopathy, stroke, rheumatoid meningitis, and rheumatoid nodules in the spinal cord.
Musculoskeletal: Osteoporosis is a common complication with RA, which can lead to increased risk of bone fractures, particularly at the femur’s neck and vertebral compression at the mid-thoracic or upper lumbar spine.
How is rheumatoid arthritis diagnosed?
Because rheumatoid arthritis is caused by multiple factors, it’s difficult for many physicians to confidently make a diagnosis, especially if the disease is at its early stage.
Two common ways they diagnose include:
Blood tests: Clinicians look for signs of anemia as well as biomarkers that indicate that rheumatoid arthritis might exist. These biomarkers include C-reactive protein (CRP), elevated erythrocyte sedimentation rate (ESR), cyclic citrulline antibodies, (anti-CCP), and rheumatoid factors.
Imaging: Combined with physical examinations, clinicians likely use X-rays and MRIs to determine where the symptoms of RA are and how much progression there is.
Do any treatments for rheumatoid arthritis work?
First, clinicians often use treatments that slow down the RA progression to the point where such progression is almost stopped and to prevent remission. In 2010, a task force of rheumatologists, other clinicians, and patients recommended such “treat-to-target” approach.
The task force was also updated in 2014, providing a more inclusive and holistic approach to patient care. This includes elements of narrative medicine, such as treating RA “based on a shared decision between patient and rheumatologist,” and the physician “should involve the patient in setting the treatment target and the strategy to reach this target.”
In other words, patients should have a say in what and how they should be treated.
Medications
DMARDS (disease-modifying antirheumatic drugs) is one of the most commonly prescribed medications because of its success rate. They target specific molecules or pathways that are involved in rheumatoid arthritis inflammations.
“DMARDS are able to work on some of these pathways of inflammation to successfully change what’s going on in your body so [the immune cells] don’t attack you as much,” said Alexis Mobley, who is a Ph.D. candidate in neuroimmunology at the University of Texas in Houston.
Mobley also suffers from rheumatoid arthritis since 2011.
“I think the one that surprised me the most is Methotrexate because that’s the first one that I was put on, and I had ever known it as a cancer drug,” she said. “I was like, ‘What? Are y’all putting me on chemotherapy? How could you?’”
Mobley mentioned that there different doses of methotrexate between cancer and RA patients, and the drug has been studied for many years with the latter group.
Other DMARDs that some physicians may prescribe include sulfasalazine, leflunomide, and hydroxychloroquine. However, a 2019 systematic review found that “there was no consistent pattern in these recommendations” on a global scale.
However, the authors mentioned that these global guidelines about DMARDs are pretty consistent worldwide. These include:
- Usage of combinations of conventional DMARDs
- Bringing different experts to collaborate on the usage of DMARDs in research and clinical practice
- RA outcomes in the last two decades have “improved significantly.” This is likely because of how guidelines have improved the quality of clinical practice.
The guidelines aren’t set in stone, and they will be updated — as they often have been — as research and clinical care progress.
“Knowing that there are non-classical pathways of getting and treating inflammation is how I understand these DMARDs work,” Mobley said.
Occupational therapy and physical therapy
Like physical therapy, occupational therapy research also finds benefits of physical activity as an effective treatment. Educational and psychological approaches, such as cognitive behavioral therapy (CBT), are also effective in managing pain, function, depression, and independence.
A combination of aerobic, strength, and meditative exercises should be used for some patients. Occupational and physical therapists should collaborate with patients to find out which types of exercises would work best for each patient.
Mobley mentioned that the future of treatments is targeting specific immune cells or proteins that cause rheumatoid arthritis and other connective tissue diseases rather than suppressing your entire immune system, like with DMARDS.
“Your immune system will still be mostly intact. You don’t have to be afraid of catching a cold or doing things that drastically change your lifestyle,” she said.
Are massages good for rheumatoid arthritis?
Many people with rheumatoid arthritis may find massage therapy can provide a huge relief, but scientific evidence does not find a strong support for it.
While a 2017 systematic review (based on seven studies with a total of 352 patients) found that massage therapy is “superior to nonactive therapies in reducing [arthritic] pain and improving certain functional outcomes,” the quality of the studies are low to moderate.
This means that some of these studies have a high risk of bias that likely favors massage over other treatments.
The authors concluded that there needs to be larger sample populations and more rigorous methods in future studies of massage for rheumatoid arthritis.
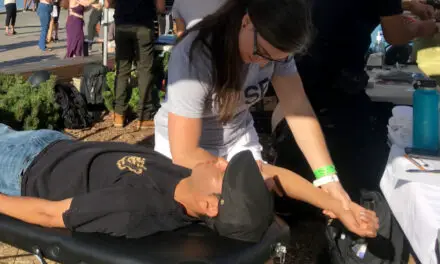
Paul Koziolek, who is a registered massage therapist for 15 years in Toronto, Ontario, and the owner of B Street RMT, said that most patients with rheumatoid arthritis have “muscle guarding,” where muscles spasm and try to immobilize the injured or painful area to prevent further injury.
“This is an automatic response to bone breaks and ligament, tendon or muscle tears,” Koziolek said. “For those with other injuries or disease processes, this can also occur to a lesser extent because of pain responses. I try to relieve this to the point where the patient has reasonable mobility and functionality for activities of daily living.”

“We cannot claim to heal these ailments, only provide non invasive relief.” ~ Paul Kiziolek, RMT. Photo: Courtesy of Paul Kiziolek
Massage therapy cannot cure or get rid of arthritic pain for good, but many people with rheumatoid arthritis may find some pain relief with massage.
While there isn’t much quality research in massage therapy for rheumatoid arthritis, the basic ideas behind how pain works can help answer how massage could alleviate pain — temporarily.
Descending modulation refers to the changes in parts of the brain that processes nociception (stimuli that signal actual or potential threat to you). These changes can pump up the pain “volume” up or down.
Different stimuli and the degrees of the stimuli that can elicit persistent pain would vary among different people. A healthy person who bumps their hand against a table might not perceive the incident as a threat compared to someone with rheumatoid arthritis.
“However, we need to remember to operate within the bounds of our scope of practice,” Koziolek said. “We cannot claim to heal these ailments, only provide non invasive relief.”
Living with rheumatoid arthritis

“It’s about riding the ebbs and flows, getting in when you can, sitting out when you can’t.” You gotta be unapologetic about it.” Photo: Alexis S. Mobley
Living with RA is tough enough by itself, but when there’s still a pandemic raging around the world, it only exacerbates RA suffers’ existing conditions.
While there appears to be no strong evidence between having rheumatoid arthritis and increased risk of getting COVID-19, many people with RA and other connective tissue diseases are not taking any chances with the possibility of getting infected with another disease on top of what they already have.
And on top of that, there are psychosocial problems RA patients face during the pandemic, including depression, loneliness, and anxiety.
When the second wave of COVID-19 was coming down last spring, Mobley felt more comfortable in going out while still taking precautions.
“I was double-masking and going out at odd times when there aren’t many people to pick up some things,” Mobley said.
But with the rising number of cases and deaths in the U.S. due to the Delta variant of COVID-19, Mobley had to discontinue working in the lab at the university and stay home — doctor’s orders.
“I kept getting sick, I kept catching colds just from one to two hours of interactions at my job,” she said. “I know I’m not the only one that are put in similar positions of continuing to quarantine at home. There are a lot of people who never really got to leave, so some people who are upset [said] that, ‘Well, I got my freedom back,’ but there are millions of people who never got it in the first place and are still doing 18 months at home just trying to stay alive.”
Despite being stuck at home, Mobley is still able to do research by having her lab assistant, who is a graduate student, do the actual lab work while she analyzes and interprets the raw data that her assistant sends her.
Coping with rheumatoid arthritis and retaining independence
Mobley suggests that RA patients should find a community to join. For her, it was going back on Twitter and looking for people to reach out to.
“Find people, find community, find ways to reach out,” she said. “I know it doesn’t sound exciting, but it’s been the best way for me.
“I’m currently on several Discord servers, and [connect] with several disabled individuals whom I can identify with. I’m on several Twitter group chats, and CreakJoints has their own little chats once a month, #CreakyChats, and I absolutely love [it].”
Other than chats, Mobley also finds watching a stand-up comedy before bed helps her cope and go to sleep.
For doing daily activities, like showering, dressing, and cooking, Mobley suggested that you should use any mobility aids that you can get your hands on.”
“I know it sounds easy like just go to the store and get a shower stool or walker, but there are several layers to that. There are some things you can’t change.
“If I can bring my stove down so I can sit and cook, I absolutely would.”
Because Mobley couldn’t stand for a long time, she adapted by cooking a huge batch of food one day and put it in the freezer so that can reheat the food for the next meal.
“It’s about riding the ebbs and flows, getting in when you can, sitting out when you can’t,” she said. “You gotta be unapologetic about it.”
Both Mobley and Davidson are part of CreakyJoints, an advocacy and support group for those living with rheumatoid arthritis. Mobley said that engaging on CreakJoint’s chats (#CreakyChats) seem to be more helpful than going to her doctor because she sees their tweets on Twitter or chat discussions that are “relevant to how she feels at the moment.”
Davidson said that taking care of herself beyond her joint pain, like exercise, having a support group, and working with different healthcare professionals.
“Educating myself, participating in research, volunteering with different organizations, attending classes,” she said. “There are so many free classes, like from the Arthritis Society and Arthritis Foundation. I took all of them.”
She later started to write and advocate for arthritis patients, which allowed her to cope. People who share her pain experience started to listen more and started to offer help. They did not dismiss her pain as being all in her head.
“It was a badge of honour because I was expressing myself rather than hiding it,” Davidson said. “I’m stuck with this feeling and coffee ain’t gonna fix it.”
Alexis Mobley is also the director of Blackimmune.org, a non-profit that showcases Black immunologists’ contributions to science from around the world. The group also provides resources to Black students and professionals for jobs in immunology and related fields.
You can follow Eileen Davidson for her updates and mini-adventures on Instagram.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.