Kyphosis refers to having too much curvature in your upper back, which can reduce range of motion in your shoulders and upper back extension. Too much rounding of the spine may also increase the risk of some joint disorders and diseases, such as fractures in the spine among older adults.
It has features commonly found in upper cross syndrome, which often ties with rounded shoulders and forward head posture. Like other types of postures, kyphosis may be one factor in causing back, shoulder, neck, and hip pain, but your pain experience can stem from reasons other than your structures, such as stress, lack of sleep, and poor mental health.
On average, many researchers consider kyphosis as having an angle of more than 40 degrees. This is measured by using the Cobb angle, which takes the most tilted vertebra in the highest and lowest point of the kyphotic curve.
But some research finds that the “normal” curve falls between 20–40 degrees. And so, we should consider that such a “normal” range would depend on several factors, such as age and gender.
So how can we make sense of what science says vs. what we experience and what we hear or read online?
Well, this article examines the relationship of kyphosis and pain, and what science says about what works (and doesn’t work) well for kyphosis.
Types of kyphosis
Not all kyphosis is the same, and so, each type would require different treatments for various symptoms.
Congenital kyphosis
There are two types of congenital kyphosis:
- Type 1 is where the arch of the upper spine and the spinal canal fails to form during the first 6–8 weeks of embryonic development.
- Type 2 is where two vertebrae don’t separate and remain fused together.
Although congenital kyphosis is uncommon, it has a higher risk of developing neurological problems at an early age.
For example:
- a 1999 study of 112 children and young adults with congenital kyphosis found that 10 of them had compression at the spinal cord that led to “spontaneous neurological deterioration.”
- One 28-year-old subject developed spastic paraplegia, which is the progression of weakness and stiffness in the legs.
- A 2015 case study from India of an 18-month-old boy found that he developed congenital kyphosis because he was missing two vertebrae in his thoracic spine (T6 and T7). His mother noticed a “swelling” in his upper back when he was six months old, even though he was normal at birth and later developed normal walking and other motor skills.
Thus, people with congenital kyphosis may often need surgery and physical therapy to prevent further developmental problems and improve how they move as they grow.
Postural kyphosis
Postural kyphosis often develops during adolescence and throughout adulthood. In most cases, the spine is normally developed but the curvature is exaggerated. This may be caused by a number of factors, such as too much sitting or standing, accidents, stress, mental health issues, and pain.
Scheuermann’s kyphosis
Scheuermann’s kyphosis is a congenital condition where there’s too much curvature between the T7 and T9 of the upper spine—sometimes at T10 to T12.
While it looks similar to postural kyphosis, the major difference is that when a person with Scheuermann’s kyphosis flexes their spine while reaching for their toes, the spine doesn’t round.
Based on a large 2011 study of more than 11,000 pairs of twins in Denmark, researchers found that there’s almost a 75% chance that men are less likely to inherit this condition than women.
However, they cautioned that some studies may “overrepresent” monozygotic twins and concordant pairs, which can affect this gender bias.
Some researchers found that bone density of the spine and hip is not a significant factor for developing Scheuermann’s kyphosis and neither was gender. They emphasized that future research should look at “new genetic and environmental determinants of this disease” beyond just X-rays and structure.
Kyphoscoliosis
Kyphoscoliosis is a hybrid of both kyphosis and scoliosis where there’s excessive curvature on both the sagittal and frontal planes. Think of the hunching posture with side-to-side curves that mimics the letter “C” or “S.”
While symptoms are similar to kyphosis, people with kyphoscoliosis are at higher risk for developing breathing problems because the ribcage is deformed in a way that restricts the lungs from expanding enough. This may cause breathing problems during sleep, which disrupts sleeping patterns.
Cervical kyphosis
Cervical kyphosis, also known as “military neck,” is where there’s zero or almost no lordotic curvature of the cervical spine. This can cause a reduction in range of motion in neck flexion and extension.
While this may cause some people to seek treatment, some evidence indicates that it’s not strongly correlated with neck pain.
Classification of kyphosis
In 2018, a group of researchers from Ganga Hospital in Coimbatore, India, started a classification system based on the curvature of the upper spine and the integrity of its structures.
Led by Dr. Shanmuganathan Rajasekaran, the team analyzed 180 X-rays and 76 patient records and classified three categories of kyphosis with each category having one or more sub-groups:
- Type IA: spine has no abnormalities with enough disc space to allow normal mobility and flexibility
- Type IB: spine has no abnormalities with some segments of the vertebrae fused together
- Type IIA: abnormalities in the front part of the spine
- Type IIB: abnormalities in the back part of the spine
- Type IIIC: abnormalities in both parts of the vertebrae with the spinal curve at 60 degrees or less (A), more than 60 degrees (B), or “buckling collapse” (C)
Abnormalities in the front often have loss of bone, disc, or both. The back part has more issues, including loss of function due to facet joint dislocation or loss of ligaments and bone.
To see how well this new classification works, 12 spine surgeons from six different Asian countries independently examined the system by evaluating 30 sets of X-rays, CT scans, and MRI scans on SurveyMonkey. Most of them were able to classify the extremes of the classification (Types IA, IB, 3C), but not so well on the remaining ones.
Causes of kyphosis
Besides being born with it, there are other factors that cause kyphosis.
Spina bifida
Spina bifida is a birth defect where the neural tube, a structure that develops into the baby’s brain, spinal cord, and other neural tissues, doesn’t fully develop or fails to close while in the womb. The most severe type of spina bifida is myelomeningocele, where there’s a fluid-filled sac in the upper spine with nerves from the spinal cord inside it.
If this is not treated early in life, people with this condition would likely adopt a hunchback posture to avoid pain. Surgery to treat spina bifida has many complications yet it may improve thoracic kyphosis for some patients.
Osteogenesis imperfecta
Osteogenesis imperfecta is a rare genetic disease that makes bones break easily with no apparent reason. Similar to the character “Mr. Glass” in the 2000 film “Unbreakable,” people with osteogenesis imperfecta produce too little or low-quality type 1 collagen that keeps the bones strong.
About 40%–80% people who have this condition have some sort of spinal deformities with kyphosis, scoliosis, and kyphoscoliosis being the most common, due to the “collapse” of the vertebral column.
Aging
Research finds that age is another factor that increases the risk of having kyphosis, but that alone isn’t enough to be blamed. For example, a group of researchers reviewed more than 50 years of research behind the potential causes and effects of kyphosis. They found that it isn’t caused by any single factor; rather, each person has a different mix of conditions that lead to having a severe hunching posture.
These include:
- degenerative disc disease
- genetic factors
- injuries and accidents
- weakness in the back extensor muscles from muscle atrophy
- weak electrical signals in muscles and nerves
Tumors
Cancerous tumors may contribute to kyphosis by the compression of the spinal nerves and other physiological processes as the tumor develops and grows.
Symptoms include hip pain and back pain, tenderness to the affected area when touched, and pathological fractures. These may cause some people to adopt a kyphotic posture in response to pain as well as stress.
Kyphosis and pain
While the posture may contribute to back and neck pain, a lot research since the 1990s showed that it may not be so. For example:
- A 1994 study of 610 women (ages 65 to 91) found that those with higher degrees of kyphosis had no greater risk of back pain or disability than those with less kyphotic posture. The researchers concluded that kyphosis is associated with decreased bone density and loss of height but “does not cause substantial chronic back pain, disability, or poor health in older women.”
- In the 1990s, Swedish physician Torulf Widhe examined 116 children’s posture and spinal mobility at ages five and six. Ten years later, he was able to follow up with 90 of them. On average, he found that the kyphotic curve had increased by an average of six degrees.Like the study with older women, having a high curve angle of the spine is correlated with reduced shoulder and spinal mobility. While occasional low back pain was reported among 38% of the children by the time they became teenagers, “back pain was not related to posture, spinal mobility or physical activity,” Widhe reported in 2001.
- A 2016 systematic review of 10 studies found that kyphosis “may not be an important contributor to the development of shoulder pain,” but like the other studies, there’s more mobility in the shoulders if the kyphotic angle is closer to normal range. Out of the 10 studies reviewed, four had a low risk of bias, three had moderate risk, and three had high risk. However, these findings are from single-session studies and haven’t been reliably replicated. “Even if the studies had reported significant differences in thoracic kyphosis between groups, it would not have been possible to establish whether the thoracic hyperkyphosis preceded the shoulder symptoms or if the thoracic hyperkyphosis was a postural adaptation to shoulder pain,” lead researcher Eva Barrett and her colleagues wrote. They highlighted that the evidence can only demonstrate “immediate effects” of reducing the curvature on shoulder pain and prevalent is this type of posture in groups with or without pain.
- In 2007, researchers from the University of Southern Denmark pooled data from 54 studies with more than 20,700 subjects found “insufficient evidence for an association” between spinal curves with back pain, degenerative disc disease, disc herniation, headaches, bone mass loss, and breathing disorders.
- In March 2020, a team of German and Australian researchers reviewed 41 systematic reviews and 11 meta-analyses and found some evidence of an association between the posture and pain, but only for a short period of time and the “findings are not consistent.” Because these studies have different ways of examining the evidence, the results are “conflicting.” Since systematic reviews and meta-analyses are supposed to be the highest level of scientific evidence in research, the authors said these reviews seem “helpful to no one [because] a simple consensus is not available.” Thus, they concluded, “there is no simple, clear link to [low back pain].”
Kyphosis treatments
Treatment depends on the severity of the curve, age, the amount of pain (if present), and any comorbidities.
This section reviews some of the major findings for common treatments and shouldn’t be used for self-diagnosis or treatment. Always consult with a qualified medical professional to find the best treatment for you.
Do back braces work?
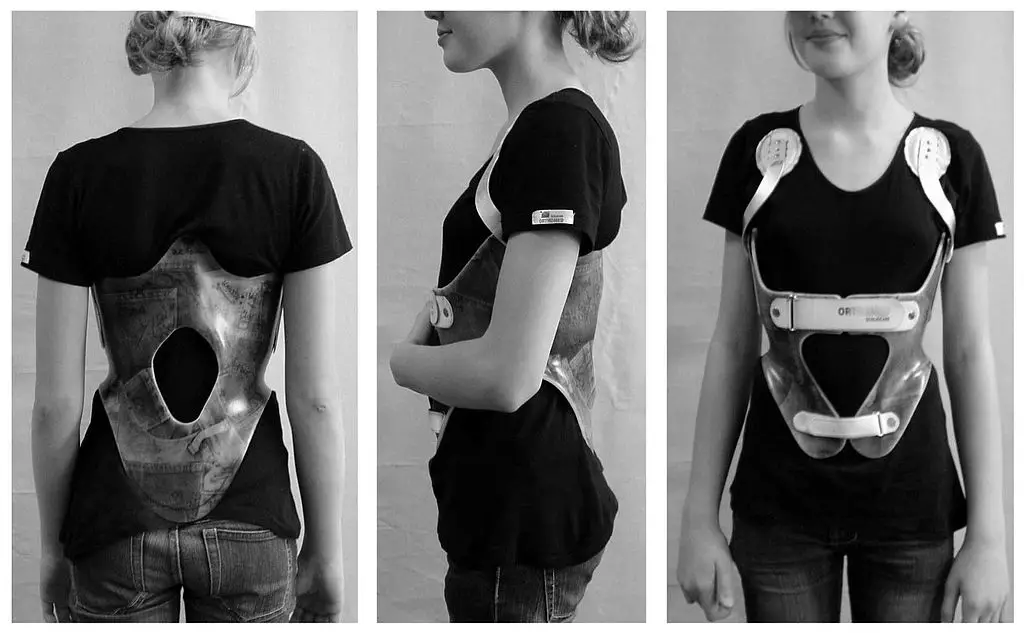
A back brace may increase the likelihood of improving kyphosis at an early age. (Photo by Dr. Weiß, distributed under an Attribution-ShareAlike 3.0 Unported (CC BY-SA 3.0))
For Scheuermann’s kyphosis, there’s some evidence that a back brace—combined with physical therapy—can reduce the curvature of the upper spine.
Historically, bracing has been shown to have some success. For example, in a 1974 study, 75 out of 223 patients who completed the trial had an average of 40% improvement in kyphosis and a 36% improvement in lordosis. But those with scoliosis had no effect.
About 12 years later at the same study location, the same researchers followed up with 120 out of 274 patients who wore the back brace since the beginning of their diagnosis and treatment. They found that 76 of them showed improvements since the beginning, 24 patients had worsened, and 10 had no changes.
Seven of the 24 patients who had worsened had a surgery for kyphosis before the study. Ten of the patients had inconsistent use of the back brace in which two of them had improvements while the others had worsened. However, a back brace treatment would work better if Scheuermann’s kyphosis is detected earlier in life.
The researchers reported that back brace treatment is “almost always successful in patients with kyphosis between 55 degrees and 80 degrees if the diagnosis is made before skeletal maturity.” It would not likely work if the angle is more than 80 degrees without surgery in patients with symptoms.
(Photos of braces for Scheuermann’s kyphosis in the 1970s.)
In 2014, Turkish researchers suggested that, for Scheuermann’s kyphosis, the back brace should be worn more than 20 hours a day for at least 18 months. When the postural correction is achieved, the time can be reduced to 12 to 14 hours a day. But they didn’t report how long patients should continue to wear one afterwards, but from the previous long-term studies, they said it’s likely that they would have to wear it for a few decades.
Exercise
Exercise may help reduce the kyphotic angle. In a 2019 systematic review and meta-analysis of 10 randomized trials, researchers found that exercise has “a large, statistically significant, effect of exercise improving thoracic kyphosis angle” but not so much for lordosis.
Strengthening exercises are likely to be more effective than stretching alone, which should be done 2–3 times a week for 8–12 weeks to see any significant improvements. But there are some caveats to this study.
Because different methods are used in the studies, such as how the angle of the posture was measured, the researchers pointed out that this may have different outcomes if the angles were measured consistently instead.
The sample sizes were small in some of the trials, and there’s also risk of publication bias. Plus, this review may apply primarily to postural kyphosis. And because strength exercises may help reduce the hunching in the long run, it probably wouldn’t hurt to do regular back and shoulder exercises. The painkilling effects of exercise may also alleviate some pain.
Surgery
Surgery should be the last option for the most severe cases. Researchers Yaman and Dalbayrak suggested that surgery “should be considered for symptomatic patients when the thoracic kyphosis exceeds 80 degrees and thoracolumbar kyphosis exceeds 65 degrees.”
Other considerations for surgery include:
- failure of conservative treatments
- rapid curve progression
They identified a few indications for surgery.
- Postlaminectomy kyphosis: Surgery should be considered for patients with several compressions or tumors in the cervical spine. Patients with cervical lordosis are at higher risk of developing postlaminectomy kyphosis than those without such neck posture.
- Post-traumatic kyphosis: Accidents, injuries, and other types of physical trauma can cause fractures, neural damage, and other problems in the spine. Yaman and Dalbayrak wrote that the goal of surgery is “to remove the existing neurological compression and bring the sagittal balance back to normal range.”
- Ankylosing spondylitis: This is one of several types of inflammatory rheumatic diseases, which affects the entire spine and sometimes other joints, including the sacroiliac joint, knee, and hips.
The goal of this surgery is to correct the chin-brow vertical angle to allow patients to look straight ahead. - Congenital kyphosis: For this type, surgery is a bit more complicated because the patients are mostly young children at age five or younger. Fusion of the posterior aspect of the spine can control the rate of changes of kyphosis as the child grows.
They warned that paraplegia might develop because of a decrease of blood supply to the spinal cord during spinal extension and compression. - Neuromuscular kyphosis: Causes of this condition include neuropathic and injury to the spinal cord, which include cerebral palsy, spinal cord injury, and syringomyelia.
The goal of surgery is to “restore spinal balance, increase the respiratory capacity, and relieve pain.”
(This is not a substitute for medical advice from a qualified healthcare professional. Consult with your health provider for your personal needs.)
Should I still try to fix kyphosis?
Other than severe forms of kyphosis that restrict movement or cause severe pain, you may not need to “fix” your posture.
We’ve already seen that anatomy alone isn’t enough to explain why we have chronic pain, yet many treatments today still focus mainly on the body parts like we’re robots.
Remember that many factors contribute to your pain experience, including our psychology and environment. Some people may have a slouched posture, but that doesn’t necessarily mean they have a disability or lack independence.
So instead of fixating on posture, a better alternative may be to seek activities that you enjoy doing regularly. Managing your well-being, such as stress, sleep quality, and social connections may also help alleviate pain.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.






