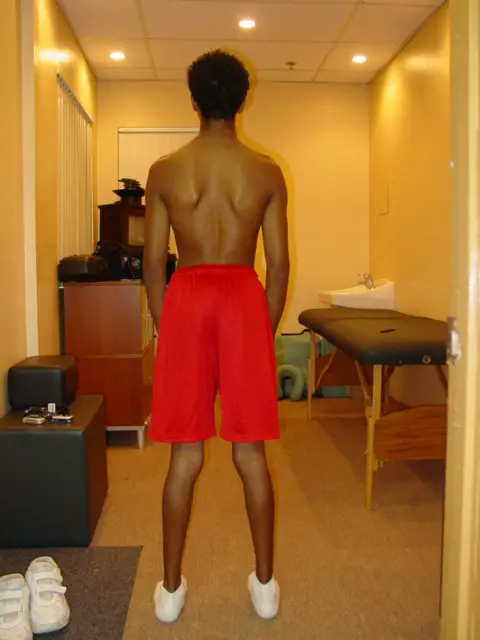
Scoliosis is an abnormal, side-to-side curve of the spine, which may originate in the bones or created by muscles pulling on the bones. It can be a single or double curve, and it’s often diagnosed among children and teenagers since their bones are easier to change and adapt than adults.
Also, scoliosis may cause excessive forward rounding of the upper back—known as kyphosis—with rounded shoulders and forward head posture. It may also cause lower cross syndrome where there are neuromuscular imbalances in the pelvis, lower spine, and legs.
Variations of scoliosis are quite common and are not always linked to pain and dysfunction. Therefore, there’s a good chance that your scoliosis may not need to be fixed if you can do your daily activities with no severe pain or disability. However, back pain may sometimes flare up and there are options for you to try to alleviate the symptoms. And that includes masasge therapy.
How massage therapy can help with scoliosis pain
Massage therapy won’t change your scoliosis, but it can give you a natural painkilling effect in reducing back pain, hip pain, and other types of muscle and joint pain. It works by stimulating certain nerves and sensory organs in your skin that reduces pain sensitivity in your central nervous system and your brain. This complex process is called descending inhibition, which is based on the gate control theory of pain.
One case study of a 63-year-old man with scoliosis and osteoarthritis found that four sessions of massage therapy over a 20-day period improved his ability to walk and reduced his pain level, which also reduced his reliance on pain medication and allowed him to ride a bike again. Keep in mind that this is just based on one unique individual and may not apply to everyone.
The downside is that the pain relief is oftentimes short-term, lasting anywhere from a a few days to a week. Depending on your income and what your health insurance covers, many people cannot afford to have a weekly session for many weeks or months.
However, massage therapy could provide a window of opportunity for you to experience that gap of pain relief, allowing you to sleep better, have less stress, and do the things you want to do without or very little pain. And so, this may cause a domino effect that can gradually reduce the severity of chronic pain.
Scoliosis symptoms
Symptoms of scoliosis can vary widely, depending on the type of scoliosis and how you got it. Some people are completely asymptomatic and find out they have scoliosis when they have X-ray imaging done for another reason.
Others may experience the following symptoms:
- back and leg pain
- numbness
- tingling
- shooting pain along the back or hips
- cramping in one or both legs.
Researchers in 2010 found that adults with scoliosis are slightly more likely than the general population to have back pain, but the degree of pain is not necessarily related to the severity of the curve or increasing age.
In severe cases, the bending and twisting of the spine can negatively affect lung and heart functions. And so, surgery may be required to increase life quality and expectancy.
Psychosocial symptoms of scoliosis can also affect your pain experience. Researchers in one study found that subjects were more likely to experience low self-esteem and depression and reported a lower quality of life related to physical health.
In another study, researchers found that people with scoliosis may experience negative psychological and social effects of this condition. These factors may be amplified if surgical treatment or bracing is required, or if the patient’s ability to participate in sports or other meaningful activities is impacted.
Types of scoliosis
There are four main types of scoliosis:
- idiopathic scoliosis
- congenital scoliosis
- degenerative scoliosis
- neuromuscular scoliosis
Idiopathic scoliosis
Idiopathic scoliosis accounts for 80% to 90% of all scoliosis diagnosis. No one really knows what causes it, but it usually starts in adolescence. Adolescent idiopathic scoliosis (AIS) is the most common type of scoliosis and is more frequently seen in girls.
Girls with AIS are more likely than boys to have a curve that progresses to more than 40 degrees, which is considered severe scoliosis. Although the cause of AIS is not clearly understood, some researchers suggested that this may occur during the large growth spurts that happen during puberty.
You probably don’t need a treatment for AIS since most cases don’t cause pain or movement dysfunction. However, some research finds that those with scoliosis may have a higher likelihood of getting back pain during old age than those without scoliosis.
Congenital scoliosis
Congenital scoliosis occurs when a person is born with some vertebrae deformity. This can be mild and require no intervention, or it can be severe which may require surgery.
While it forms within the first six weeks of embryonic development, the causes of congenital scoliosis are not clearly understood but are likely numerous and may include both genetic and environmental factors. It is not hereditary.
The bones may fail to form properly, separate properly, or both. This tends to happen at more than one spinal level and often more on one side. In severe cases, you may have fusion of the ribs and compression of the rib cage on one side, leading to problems with breathing and heart function.
Degenerative scoliosis
Degenerative scoliosis happens along with degenerative conditions of the bones and joints of the spine, such as degenerative disc disease, osteoporosis, facet disease, or arthritic changes.
The spine is made of vertebrae which stack on top of one another like bricks. If this support becomes damaged or breaks down on one side, the spine above will deviate. Thus, your body may adapt by curving in a way to maintain balance and keep the head on top of the body.
Degenerative scoliosis can create further problems as the body is forced to accommodate loads in new ways, and your muscles have to work harder to adapt to degenerative structural changes. Such changes may cause pain as more stress is applied to the spine when you move or maintain your posture when you sit or stand.
Neuromuscular scoliosis
Neuromuscular scoliosis affects the ability of your nervous system to control the muscles around the spine. This can be caused by:
- cerebral palsy
- Jeune syndrome
- Marfan’s syndrome
- spina bifida
- muscular dystrophy.
Researchers have found that the incidence of scoliosis ranges from 20% to as high as 64% in cerebral palsy patients. Neuromuscular scoliosis can also happen after a spinal cord injury.
A 2013 review suggested that this type of scoliosis is far more likely than AIS to be severe and progressive and contribute to further health problems.
Adaptive scoliosis
Adaptive scoliosis can happen when the muscles are adapting to scoliosis lower in the lower back, a tilted pelvis or leg length discrepancy. It may also happen when you’re experiencing severe chronic pain for years.
Athletes can also get adaptive scoliosis, especially those who play sports that require powerful, repetitive movements in one direction or of one limb, such as volleyball or baseball. But no one knows whether the imbalanced muscle usage leads to scoliosis or if there’s a higher prevalence of scoliotic people in certain sports.
Can surgery fix scoliosis?
The short answer is: it depends. Surgery is generally for those with a curve of greater than 40 degrees, or whose scoliosis is progressing and creating health problems.
Two systematic reviews of surgery for AIS done in 2009 and 2017 found no benefit for this population versus allowing scoliosis to follow its natural course or applying conservative treatment approaches.
Both reviews stated that the traumatic and invasive nature of surgery must factor patients’ long-term outcomes and should be suggested as a last resort.
Another review examined surgical outcomes for adult scoliosis patients and found there’s a lack of standardized outcome measures, making it difficult to draw general conclusions from the research. The researchers found post-surgical improvements in disability, physical, social, and mental health measurements. However, complications occurred in as many as 40% of the cases. They concluded that the benefits should be seriously weighed against the surgical risks.
Surgery may include:
- removal or shaving of bone
- fusing of vertebrae to limit movement
- insertion of hardware to provide support and guidance to growing structures, especially for children or teenagers.
Older surgical approaches, like the insertion of Harrington rods, resulted in a rigid, straight back and limited range of motion. Over time, surgical methods and technology have been adapted and greatly improved since the mid-20th century. Newer approaches, like Anterior Vertebral Body Tethering, offer surgical options that don’t decrease mobility much.
In cases of neuromuscular scoliosis, researchers found that surgery may contribute to increased family and caregiver satisfaction rates, in addition to providing added stability to the patient.
Scoliosis treatment
Between observation for the mildest cases and surgery for the most severe, there are many non-invasive approaches for managing scoliosis.
Electrical stimulation
A 2005 systematic review found no evidence to support the effectiveness of this treatment approach. However, Polish researchers in 2009 found that two hours per day of such therapy for more than 24 months was effective at decreasing progression rate in those with a scoliosis of less than 20 degrees.
The study compared results with an exercise control group, as well as a group which received nine hours per day of electrical stimulation. Interestingly, they found no difference in outcomes between those who received two and nine hours of treatment per day.
Manual therapy
Massage therapy, chiropractic, and osteopathic care have long been used to manage pain. While these disciplines historically lack well-conducted research to back up their claims of effectiveness, this doesn’t mean they are never helpful in individual cases.
A 2008 systematic review found that there was simply no good evidence that manual therapy can effectively manage scoliosis. However, the study is based on three qualified trials, and they all examined mixed manual therapy approaches to scoliosis treatment.
In 2019, a team of researchers broadened the scope of the review to include any relevant published English language research, regardless of quality, including case studies. Case studies do not replace higher quality and larger scale objective research, but these “n=1” studies may provide some insight into how manual therapies may support scoliosis management.
They found that all case studies showed improvement in all measured parameters while observational studies had mixed results. One randomized-controlled trial found no benefit in manual therapy for improving trunk shape and spinal flexibility.
Ultimately, the researchers still concluded that there was no high-quality research from which to draw any conclusions whether manual therapy works or not. But they did note that the evidence provided some basis to justify further study since there may be potential benefits of manual therapy as part of a treatment plan.
Physiotherapists and other health care providers often work together to use conservative care of scoliosis and its symptoms. Treatment approaches may incorporate active exercises, manual therapy, taping, bracing, medications, and mental and occupational health care and support.
Amberly Horton, a registered physiotherapist in Grimsby, Ontario, encourages that manual therapists consider both structural and functional aspects of scoliosis in assessment and treatment.
“This means looking at the position and shape of the vertebrae, as well as the movement patterns, body awareness, general strength and flexibility, and strength in muscles that contribute to posture,” Horton said. “The role of physiotherapy in treating scoliosis is to retrain the brain and body to slow the curve progression and manage the patient’s pain.”
Horton emphasizes the importance of working with each patient to assess and meet their individual needs and goals, and aiming to support them in living successfully with scoliosis.
Keep in mind that treatment should not only be aimed at addressing the structural issues but also managing the unpleasant symptoms. The curve itself may not be the problem, but rather a symptom or even an adaptation.
Note: Do not replace the information in this article with the advice of a qualified medical professional. Consult with your physician to determine the appropriate care.
Do braces for scoliosis work?
Bracing has been used to treat AIS for many years, which is used to control and direct the growth of the spine and ribcage among children and teens. It’s also used when the scoliosis is progressing, has exceeded 40 degrees, and/or has progressive and worsening symptoms, such as pain.
A 2019 meta-analysis of seven studies found that bracing is a safe and efficient treatment for AIS compared to no specific treatment. But there was a lack of follow-ups so no one knows how well these braces work in the long run.
They also found that those in the bracing had “higher” quality of life but these patients have their own challenges, such as pain, skin irritation, and problems in lung and kidney function.
There are five main types of braces:
- Boston brace
- Milwaukee brace
- Charleston bending brace (“nighttime brace”)
- Cheneau brace
- Lyon brace
The Boston and Milwaukee braces are similar, except that the Milwaukee brace has a neck ring for added stability.
The Charleston bending brace is intended only for sleeping in, whereas the other two are intended to be worn 23 hours per day. This dosage of bracing has been found to be effective.
The Cheneau brace is designed to overcorrect and force the trunk into an opposite position to that of the scoliosis.

A sample of the types of back braces available. (Image credit: MDPI, distributed under Creative Common license, Attribution 4.0 International (CC BY 4.0))
These braces are usually made of rigid plastic, custom molded to the patient’s body. They’re designed to put pressure on the convex portions of the scoliosis and to provide space in the concave area. Over time, spinal growth will fit the brace, and the curve will be reduced.
Because you have to wear the brace nearly all day and perhaps for many years, some companies have designed the brace with more aesthetic appeal and flexibility to adapt to each person’s body and movement patterns.
Does scoliosis cause back pain?
Because back pain is caused by many factors—not just one—it’s hard to determine if scoliosis is a primary cause of back pain. But research can help you sort that out.
One research of more than 1,300 elderly people with scoliosis found that they’re more likely to experience back pain than those without scoliosis. Interestingly, they found no correlation between the degree of the scoliosis and the severity of the symptoms. The researchers also found that back pain was more prevalent in those who had received surgery to treat scoliosis.
In another study that examined the natural history and long-term treatment outcomes of AIS, the researchers found that although back pain is more common among teenagers with scoliosis, there may not be a significant difference in the severity or duration of back pain episodes when compared to a non-scoliotic sample.
As you can see, back pain is caused by many factors, influenced by physical and psychological factors. People who tend to catastrophize pain are more likely to experience higher pain severity regardless of what kind of spinal curve they have. Thus, you should consider the role of mental health support and psychology in scoliosis pain management.
Scoliosis exercises
Exercise for scoliosis can improve your physical and psychological health, which can decrease the symptoms of scoliosis. These include:
Bird-dog stretch (with resistance)
Double leg abdominal press
Plank
Pelvic tilts
Cat and camel
Standing wall
Child’s pose
Seated twist
Kneeling hip flexor stretch
Seated butterfly stretch
Supine rotation stretch
Schroth Method
The Schroth Method is an exercise program that tries to gradually move the spine to a more neutral position by rotating, elongating, and stabilizing the vertebrae and the muscles and tissues around it. Researchers have found some support for this specific method, although they caution that such support is limited, and therefore these exercises are best used in combination with other conservative approaches.
Otherwise, exercise could slow down the progress of scoliosis, decreasing Cobb angle, and reducing the need for a brace.
Final thoughts about scoliosis
I have consistently experienced low back pain on one side since my late teens. Who knows if this is related to the curve in my back? The idea that it was, was reinforced to me many times. Perhaps the negative messaging about pain has also played a role in the presence of pain.
It seems possible that what I thought for 20 years was scoliosis may actually fall within the parameters of normal structural variance, although there’s a mild congenital malformation of my spine. If I do have a mild scoliosis, as defined by a 10 degrees or greater curve, I don’t need a diagnosis because I already know that, for me, being a little crooked is really not that big of a deal anyway.
And if it ever were to feel like a problem, I know there are lots of good options available for safe, effective, and non-invasive symptom management.

Frances Tregurtha, RMT
Frances has been a registered massage therapist in Ontario, Canada, since 2000, and she is working toward completion of a diploma in manual osteopathic practice.Her clinical background includes private practice, long-term care, and palliative work, as well as motor vehicle injury rehab and work with traumatic brain injury patients.
She currently works in two clinics, one of which is a multidisciplinary setting focusing on women’s health and pediatrics.
Outside of work, she can be found with her family and dog, cooking, gardening, camping, hiking, beach-going, and squeezing in a moment here and there for yoga and a scenic jog.