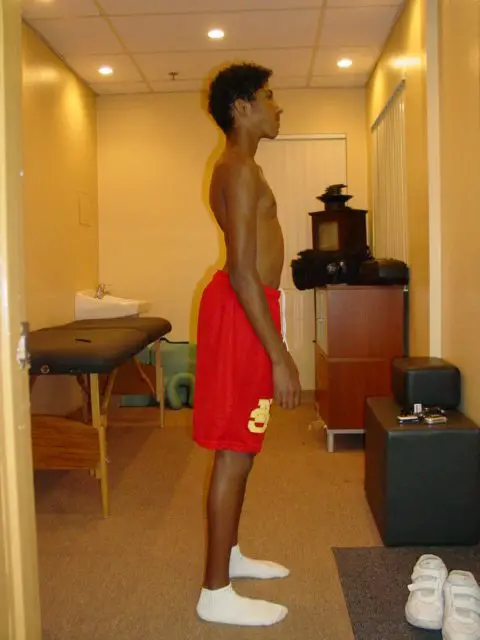
Lordosis (also called “swayback”) is where your lower spine curves inward excessively. Such curve functions as a shock absorber, adapting to movement and load and keeping your body stable.
While having spinal curves is natural and beneficial, having too much low back curve may cause health problems. But based on the body research on lordosis, pelvic tilts, and other types of posture, it’s probably not as bad as you think.
Lordosis vs. kyphosis and scoliosis
Some people get confused with the difference between lordosis, kyphosis, and scoliosis, which refers to the curves of the spine.
- Lordosis is having too much inward curve in the lumbar and cervical spine.
- Kyphosis is where your upper spine curves outward excessively, causing your ribcage to curve back. This can cause forward head and rounded shoulders.
- Scoliosis is the side-to-side curve or rotation of your spine, which may often contribute to back pain, especially among children and teens.
Lordosis symptoms
The most obvious visible symptom is the lower back arch that sometimes exaggerates the shape of the buttocks because the pelvis is rotated forward. But many people believe that this causes back pain, hip pain, and neck pain.
However, research has shown that if you were to look at the lordotic angle alone, you won’t likely be able to tell who has low back pain or not. That’s because people can have back pain regardless of the spinal curve.
In fact, having less lordosis is associated with higher likelihood of having low back pain. Some researchers suggested that this may be an adaptation to avoid pain.
What causes lordosis?
Cervical and lumbar lordosis are thought to be caused by some common factors, such as spondylolisthesis (a vertebra “slips” forward onto the bone directly below it), obesity, osteoporosis, and discitis (inflammation of the space between vertebral discs). However, research has shown that these factors do not always predict whether you’ll get back or neck pain.
Spondylolisthesis
Spondylolisthesis is when your vertebra “slips” forward onto the bone directly below it. A 2020 study found that people with this condition are more likely to have higher degrees of lumbar lordosis and pelvic tilts than those without spondylolisthesis.
The researchers concluded that the posture “may be a compensation mechanism” to reduce pain and maintain balance.
Another research from Japan found that having spondylolisthesis is more likely to contribute to leg pain instead of low back pain.
Obesity
Obesity may affect the degree of the lordotic curve, including children. Having too much belly fat can increase pressure on the lumbar facets of the vertebrae and shift the weight to the front of the body.
Osteoporosis
Osteoporosis is the gradual loss of bone mass, which increases the risk of fractures. Some people believe that such loss causes the lower spine to weaken and pull your pelvis forward, but this isn’t quite true.
A 2008 Greek study of 112 women compared those with either osteoporosis, osteoarthritis, or both diseases with healthy controls. The researchers did not find significant differences of lordotic curves among all the women.
Another study in 2013 of more than 250 women found a weak, but significant, association between lumbar lordosis with bone mineral density. However, the risk of osteoporosis in the thoracic spine appears to be great among post-menopausal women with kyphosis.
Discitis
Discitis is the infection of the space between the vertebrae, which affects mainly in toddlers and children. Research does not find a strong association with lumbar lordosis and discitis. In fact, the lack of lordosis may also be an adaptation to reduce pain.
Accidents and falls
A car accident or a fall may change how your neck is curved. Research finds that most people who suffer a whiplash adopt a forward head posture with a lower cervical curve. But having less curve doesn’t mean you’ll get neck pain. Some people who had a car accident and a reduced neck curvature reported to have no neck pain.
“Has anybody ever stopped to think that maybe this curvature of your spine is much more driven by nature than it is by nurture? Is the lordosis and kyphosis in your spine actually a factor of genetics?
“We see people with genetically longer torsos or longer legs. We see people that are genetically taller and genetically shorter. We see genetic components to eye color and hair color. But when we look to the structure of a persons spine, all the sudden it’s 100% about their activity and sitting posture???” ~ Dr. Jarod Hall
Lordosis exercises
While there’s a weak association between lordosis and low back pain, you might find some pain relief from exercises that target the lumbar and pelvic region.
Science indicates that strength training may be better for changing both kyphotic and lordotic curves, but the amount of change is too small to have any significance.
Generally speaking, the researchers recommend strength training two to three times a week for eight to twelve weeks to see any improvements in spinal curvatures.
Sample exercises include:
Ball reverse hip extension
This exercise strengthens your glutes and core muscles, which may help reduce the lumbar curvature.
- Lie on a stability ball on your stomach with your forearms on the floor. Your body should be shaped like the yoga pose downward dog.
- Exhale as you raise your legs up as high as you can while keeping your legs together. You should feel your glutes clench together like you’re holding a $100-bill between your buttocks.
- Stop raising your legs if you feel your lower back begins to arch.
- Hold this position for one to two seconds, and lower your legs to the ground until your toes touch the floor
- Repeat for 10 to 12 reps.
Glute bridges and pelvic thrusts
Although both exercises can help reduce the lordotic curve, they also help strengthen and increase power in your glutes.
Deadlifts
Deadlifts target your glutes as well as strengthening your torso. It can also reduce low back pain while increasing low back strength and endurance if done properly with the right amount of recovery between exercise sessions.
- Stand with your feet about shoulder width apart with the barbell in front of you.
- Bend your knees slightly as you reach forward to grab the barbell with your hands about shoulder width apart.
- Exhale as you push your hips forward as you straighten your torso. The exhalation automatically braces your abdominal muscles to stabilize your body as you lift.
- Tighten your glutes as you hold the standing position for one second before you lower the weight back to the ground.
- Bend your knees as you lower the weight.
If you’re new to this exercise, work with a qualified personal trainer for a few sessions before doing it on your own. You can also do this with kettlebells and dumbbells.
For back pain relief, almost any kind of exercise would work, and none are “better” than another. It should be something that you enjoy and can do consistently.
Take away
As you can see, pain is caused by many factors, blaming any single piece of anatomy or posture can make you miss out on other things that may also contribute to your pain, such as lack of sleep, stress, anxiety, and pathologies.
For example, a 2013 study found that age, gender, body mass index, ethnicity, and sport, “may affect the lordosis angle, making it difficult to determine uniform normal values.” They emphasized that normal lordosis “should be determined based on the specific characteristics of each individual.”
So if you have lordosis, have no pain, and can go about your day with little or no trouble, you may not need to fix your posture. There are many causes of lordosis and not all of these cause back or neck pain. In fact, your lordosis might not be causing any problems at all.
But it doesn’t hurt to check with your healthcare provider if you’re worried about your posture.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.