While the Beighton score is a “standard” assessment to diagnose whether you have joint hypermobility or Ehlers-Danlos syndrome (EDS) and similar disorders, recent research questions its validity and reliability of the scoring system.
In 2020, British and South African researchers found inconsistencies of the “hands on floor” part of the Beighton score assessment to determine whether some children are truly hypermobile or not.
In 2021, British researchers, led by Ph.D. student Sabeeha Malek from the University of Warwick, questioned the Beighton score’s validity since they found glitches in the scoring system that can make clinicians overlook generalised joint hypermobility in patients, which in turn, may be preventing patients from receiving their EDS diagnosis.
“My personal perspective is that the standard understanding of hypermobile joints in relation to EDS is outdated,” Malek said, “and therefore, so is the expectation that hypermobility scores amongst EDS patients should be consistent.”
She emphasized that the degree of joint hypermobility is often mistaken as a sign of the degree of “abnormal” connective tissue disease.
“Or in other words, the assumption that someone with more severe hypermobility has a more severe case of EDS and/or experiences more debilitating symptoms. We know this is not the case,” Malek said.

Ph.D. student Sabeeha Malek from the University of Warwick questions the status quo of the Beighton score. Photo courtesy of Sabeeha Malek.
There are other typical factors that influence hypermobility, such as prior stretching, body temperature, menstrual cycle stage, and muscle mass and tone. And so, someone could be hypermobile yet these factors mask their underlying hypermobility. Thus, these patients might be overlooked and could be prevented from receiving their true diagnosis.
“The reason there are inconsistencies with hypermobility scores amongst patients is because so many of these non-disease related factors influence it,” Malek said. “I believe it has long been past the time since we considered these ‘inconsistencies’ as unusual.
“In fact, they are completely expected and, to a certain extent, clinically unremarkable.”
What is the Beighton score and how is it calculated?
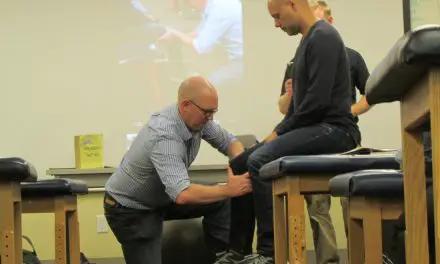
The Beighton score is based on a 9-point scale that is based on five joint assessments where the score ranges from 0 to 9. The first four assessments are evaluated bilaterally.
- Passive dorsiflexion of the fifth finger (pinkie) to see if it can move beyond 90 degrees
- Thumb touches the forearm flexors
- Hyperextension of the elbows
- Hyperextension of the knees
- Both hands touch the floor while the knees are fully extended
The clinician scores one point for each assessment that the patient can do. The cut-off point is scoring a 5 for adults and a 6 for children, but this system can be problematic since there’s so much variation and factors that influence what’s considered hypermobility, EDS, or otherwise.
Developed by two physicians, Cedric Carter and John Wilkinson in the mid-1960s, the scoring system was first used on 145 girls and 140 boys in the U.K. who showed symptoms of joint laxity and hypermobility.
In the late 1960s, British geneticists Peter and Greta Beighton expanded the scoring system which gave its namesake today. While studying joint and bone disorders in South Africa in the early 1970s, Greta proposed the 9-point scaling system that is still used today but remained unchallenged until recently.
In November 1972 at the Heberden Society in London, they presented their research of more than 1,000 Tswana children where they emphasized that the fifth finger dorsiflexion test is the most “valuable and sensitive technique.”
According to Prof Rodney Grahame, the godfather of #hypermobility, who knew the Beightons, it's "BITE-on", rhymes with Brighton (as in the old criteria for #JHS). And he says having the Score & Criteria one letter apart was the biggest mistake of his career 😆.#EDS facts
— Emma 💉💉 Reinhold😷 #BLM (@DrEReinhold) October 6, 2021
Is the Beighton score really valid and reliable?
Despite its popularity and legacy, the Beighton score may not be the Holy Grail to determine if someone has EDS or joint hypermobility.
For example, going back to the “hands on floor” study, 35% of the 460 South African children were identified as hypermobile, but only a fraction of them (about 8%) can touch their hands on the floor.
Corten et al. wrote that “no clear universal cut-off score is defined to identify hypermobility in children and adults” and the hands on floor item “does not add additional value to the Beighton score in children of Black African and mixed ancestry.”
While a 2020 systematic review found that the Beighton score is a “reliable clinical tool” because of the consistent findings among individual and different clinicians, it doesn’t mean the tool itself is valid.
“In scientific terms, validity and reliability are very different things,” Malek explained. “Validity tells you if a diagnostic test can correctly identify the disease, whereas reliability tells you if the diagnostic test consistently produces the same result in the same patient.
“This distinction is really important because you might have a reliable tool that always produces the same result in the same patient, but if that result itself is often wrong, then I’d argue it’s not a very useful diagnostic tool!”

A recent review, led by Ph.D. student Sabeeha Malek (l), questions the validlity of the Beighton score. Malek with Dr. Emma Reinhold (c) and Dr. Gemma Pearce who co-authored the study. Photo courtesy of Gemma Pearce.
Rethinking about the Beighton score
The inconsistent findings and observations of hypermobile and EDS patients in both research and practice has led Malek to scrutinize the status quo.
Malek, who also has EDS, sifted through the EDS literature while she was pursuing her Master of Science degree in biomedical science. She wanted to zero in on the research behind the Beighton score.
“I soon connected with Dr. Gemma Pearce and Dr. Emma Reinhold who were incredibly supportive of my work and helped develop my [Masters of Science] assignment for publication,” she said. At the time, Pearce was already leading a series of research on hypermobile EDS and related conditions.
“I was working with Emma on some research, too, and introduced [Malek] to the team because I thought [Emma’s] experience and knowledge would be a useful addition,’’ Pearce said. “After that when Sabs was successful in securing her doctoral funding, she did an internship with me at hEDStogether. We wanted to make sure that this important Masters work was published.”

“I, myself, have the condition and am lucky to be in a position where I can carry out research while having a deeper understanding through my own lived experience.” Photo courtesy of Dr. Gemma Pearce.
Pearce’s research focuses mostly on hypermobility and how it’s diagnosed. She found that it’s a typical issue that pops up not only in research, but also among patients, charities, and clinicians.
“Providing an in-depth look at the purpose that the Beighton Score should and shouldn’t serve was an important part of moving this field forwards,” Pearce said. “I, myself, have the condition and am lucky to be in a position where I can carry out research while having a deeper understanding through my own lived experience.”
Malek’s current Ph.D. supervisor, Dr Darius Köster, who specializes in cell biomechanics, agreed to oversee her doctoral research on EDS. Malek wanted to end how heavily clinicians rely on subjective criteria for EDS diagnosis.
In her first year of research, Malek theorized that it’s the collagen that fails to attach to fibroblasts — cells that secrete collagen proteins that provide the structure of connective tissues — not because of the collagen itself.
“We are now working in the lab to develop a test for membrane-bound collagen and we are also investigating several aspects of this pathomechanism further,” she said.
Dr. Emma Reinhold, who developed an Ehlers-Danlos syndrome toolkit for the Royal College of Physicians in the U.K. and co-authored the critique with Malek and Dr. Gemma Pearce, said that people with symptoms of EDS, such as having super-stretchy skin, “failed to meet diagnostic criteria” because their Beighton score was “too low.”
“These people often had many other joints which were hypermobile, just not the ‘right ones’,” Reinhold said. “Because there are so many barriers to diagnosis anyway, we wanted to closely examine the evidence behind the use of the Beighton score alone in the 2017 criteria. We believe that diagnosis is so important to prevent further damage and access safe and appropriate care.”

Dr. Emma Reinhold assisted in the research by interpreting the data that Sabeeha Malek had gathered. Photo courtesy of Emma Reinhold.
The research team isn’t dousing the Beighton score with kerosene and tossing it into the dumpster fire, but assessment and diagnosis should not be based heavily on a number at all.
“What we are suggesting is that if a patient doesn’t reach the threshold score on Beighton, but you as a clinician are suspicious that they may have a hypermobility-related or collagen disorder, it is important to examine other joints and to consider the patient holistically,” Reinhold said.
While clinicians can still use the Beighton score to confirm joint hypermobility, consider that the scoring system is biased to the upper limbs.
“[The Beighton score] cannot be used alone to exclude generalised joint hypermobility,” Reinhold said.
Future of Ehlers-Danlos syndrome research: beyond the Beighton score
Traditionally, EDS — like most connective tissue diseases — are often classified as “rare,” but more recent research found that it’s more common (at least in Wales) in recent years.
Pearce mentioned that a 2017 systematic review that examined the methods of assessing joint hypermobility served as their “launch platform” for their current review.
“The current field is evolving and this publication has been really important to help it continue to move forwards,” she said. “We have had great discoveries and new understanding over the last few years. As researchers, we work together with charities, healthcare professionals and people with the conditions to ensure that this field develops on in a meaningful way.”
In many cases, people with hypermobile EDS were lumped together with those with hypermobility spectrum disorder — a generalization of various types of joint hypermobility where the symptoms don’t entirely fit with hypermobile EDS.
“I think we need a truly multi- and inter-disciplinary approach to understanding EDS and to identify all the factors involved in causing tissue laxity,” Malek said, referencing that other fields of cell biology are needed, such as cell biomechanics and cell adhesion.
“For example, there have not been any studies (to my knowledge) that have looked for any irregular molecular or cellular changes in EDS connective tissue when it is stretched,” she continued. “This would be quite an important approach to help determine if certain factors contribute to the properties of lax or fragile connective tissue, yet this area of research remains unexplored.”
Malek, Reinhold, and Pearce are part of hEDS Together based in the U.K. They dedicate their research in hypermobile EDS and other types of hypomobile joint disorders.
“[We often] find it is those who actually lay hands on people who are best placed to suspect these important conditions, as well as to make a huge improvement in people’s quality of life,” Reinhold said. “There is so much evidence of underdiagnosis both in the literature and anecdotally, along with increasing evidence of the interventions which make an important difference once a diagnosis has been made. That’s what we are all about.”
“Regardless of whether this field expands in the way it should, I’m still excited to have led the way into this new era of research,” Malek said, “and I am hopeful that this field will produce many more discoveries to improve the diagnosis and care of hypermobile and EDS patients.”
Follow their updates and research adventures at hEDStogether and on Twitter: @hEDStogether.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.