Should you be concerned about the effects of lactic acid build-up in your muscles? If lactic acid really does what some people say it does, then you probably don’t want that substance anywhere near your muscular system.
It’s an acid. It burns, which you can feel directly, and it causes damage, which you experience as muscle fatigue or soreness. If you keep going long enough and produce enough lactic acid, then you “hit the wall.” Your body runs out of steam, and you can’t go any further.
If lactic acid does that, then it’s a bad thing, even if the effects are only temporary. But that’s a really big “if”—is it true what they say about lactic acid?
Many people have invested in the myth that massage can squeeze lactic acid out of muscles that they are reluctant to take on the job of aligning the narrative with current scientific evidence. If massage therapy is to remain relevant in the COVID-19 era, practitioners must realize their potential as an actual healthcare professional.
What is lactic acid?
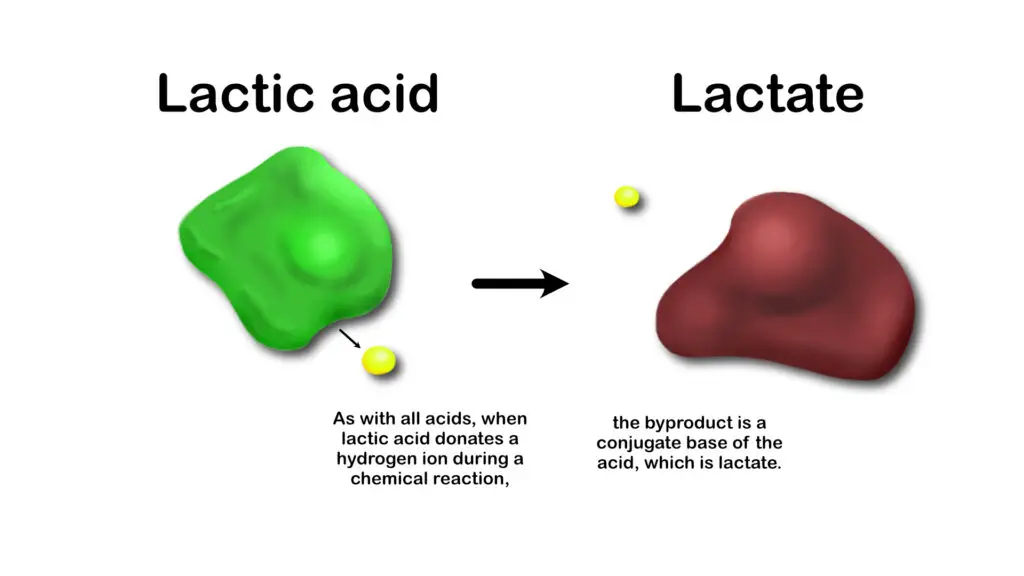
Lactic acid is an organic (carbon-based) acid found in many different natural processes. Like the words galaxies, the lactate ion, and lactation, its name shows its close connection to milk.
Sour milk is where the Swedish chemist Carl Wilhelm Scheele identified it as a specific chemical compound in 1780. Its association with food continues to this day, where that sour taste is valued in foods ranging from yogurt to sourdough bread.
The closely-related chemical lactate is in the fluids given to trauma patients being treated for blood loss until they can rebuild that capacity on their own. It also appears to be a critical component in brain development and metabolism in multiple species, including humans.
Lactate is very important in muscle physiology because exercise causes your muscles to produce it from glucose and to use it for energy. But it’s lactate, not lactic acid as many people still believe, it carries out that metabolic function.
[Video on lactate vs. lactic acid]
So does massage therapy “release” lactic acid?
Massage therapy does not get rid of lactic acid in a normal, post-exercise situation because there’s no persistent buildup of lactate. Massage, however, may be beneficial after you exercise to stimulate muscle blood flow perfusion (at rest the muscle fibers are only intermittently perfused), which may help with the healing and repair of damaged muscle fibers.
In people with limb ischemia, such as may occur with peripheral artery disease, limb edema and vascular insufficiency there may be some buildup of lactate in muscle and other tissues.
Massage therapy has much more benefits than “getting rid” of lactic acid, which is physiological implausible. It helps decrease stress and symptoms of depression and anxiety, particularly for cancer patients.
Given what we know about lactic acid, glucose metabolism, and human touch, there’s no need to tell patients and clients that massage therapy can remove lactic acid or “toxins.” Oftentimes, providing comfort, relaxation, and less pain is why they seek massage therapy.
Does lactic acid cause muscle soreness?
For about 100 years, people have correctly associated lactic acid and lactate with exercise. However, the relationship between moderate to high-intensity exercise with muscle fatigue and muscle soreness has turned into lactic acid myths. In the absence of better information, like the lack of knowledge, it was easy to pin the blame on lactate, but now we know that lactic acid has received a bad rap.
The soreness that we often get from exercise and sometimes after a massage is not caused by lactic acid buildup in muscles, nor is lactic acid responsible for post-exercise muscle spasms and delayed onset muscle soreness, muscle fatigue, or tight muscles.
A lot of research published in the past 30 years has shown that each of these myths is, in fact, a myth. Lactate and lactic acid do not contribute these effects. We know that these “exercise” symptoms are real, but they are due to other causes. These effects remain highly treatable with physical therapy and massage therapy.
But what causes the muscle burn during exercise?
Exercise scientists have known that lactic acid is not to be blamed for muscle soreness that you get after exercise. While no one really knows what causes muscle soreness, the best explanation so far is that the microscopic tears that you get from exercise cause inflammation in the muscles and surrounding tissues, which likely increase pain sensitivity in the nerves and even your brain.
But this is an adaptation to exercise, which means that when you recover from the soreness, the next workout sessions will less likely to cause the same degree of soreness as your first one.
How does your body “get rid” of lactic acid?
Lactate is not a metabolic waste product or a “toxin,” even though this may seem to be the case because it’s released by contracting muscles during exercise. Rather, we know that lactate is used as fuel in the mitochondria of contracting and recovering muscle to generate ATP.
We also know that lactate released into the blood from contracting muscle is taken up by other cells in the body including brain, liver, red blood cells, and non-contracting muscles. Lactate taken up by these cells is oxidized, (i.e. lactate is a valuable metabolic fuel that is not to be wasted). While some lactate is lost in the urine with very high intensity exercise, this is an exception. The body retains lactate and uses it. In fact, lactate is preferred over glucose as a fuel source, even in resting muscles.
Because of the mechanisms for lactate disposal in the body, lactate doesn’t linger very long after you stop exercising or cool down. Even with very high intensity exercise lactate concentrations return to pre-exercise resting levels within 90 minutes.
Therefore, there’s no buildup of lactate in muscles—nor an elevated blood lactate concentration—in the hours and days after exercise when we may experience muscle pain and soreness, cramps, twitching, and muscle damage. For the most part, these ‘effects’ are the result of mechanical damage caused by the strength of muscular contractions and chemical damage caused by reactive oxygen species (ROS).
ROS are produced in the mitochondria of cells when mitochondrial respiration (oxidative phosphorylation) is elevated as occurs with moderate to high intensity exercise. They react with cell membranes, and other elements within cells, causing damage to the membrane and other structures including the contractile apparatus itself.
The amount of damage is proportional to the intensity and duration of exercise and is most notable in untrained muscle. The damaged muscle fibers leak molecules (i.e. creatine kinase (CK) into the extracellular fluids and blood). Some of the small cytokine molecules stimulate pain-sensitive nerve endings in muscle, causing the pain that is associated with intense exercise or with delayed onset muscle soreness.
[Video on how cells metabolize lactate]
Is there a supplement that helps reduce lactic acid?
Sodium bicarbonate is the main supplement that has been used successfully to increase the rate at which muscles release lactate into the blood, thus reducing the buildup of lactate in muscle cells during exercise. The research also shows that bicarb supplementation supports the performance of short-duration (less than three minutes) high-intensity exercise.
A recent systematic review of 189 research studies of 2,019 subjects—mostly young male and female adults who are non-athletes—reported that bicarb supplementation supports the performance of short-duration (less than three minutes) high-intensity exercise. When the analysis is performed using only female subjects, the same result of enhanced exercise capacity was obtained.
While the systematic reviews do not comment on lactate, it’s known that the blood alkalosis caused by bicarb supplementation enhances muscle lactate removal. This appears to be beneficial for contracting muscles, and lactate in the blood is rapidly taken up by most other cells of the body as metabolic fuel.
There are no supplements that are able to promote lactate loss after exercise because lactate is very easily and quickly disposed of by most cells of the body, which use lactate as metabolic fuel to produce ATP. Other supplements containing sodium citrate or other weak acid salts of sodium work in a way similar to that of bicarb.
Check with your healthcare provider before you take any of said supplements. Do not substitute this for your medical advice.
Where did the lactic acid and massage myth start?
It turns out that the myth behind lactic acid’s effects is like a game of “Telephone.” It has been repeated from person to person, often getting tweaked in the telling. But the original message came from an experiment where the scientist was wrong about what he actually saw.
The German biochemist Otto Meyerhof was awarded the Nobel Prize in Physiology and Medicine in 1922 for his work on cell physiology. He examined what was going on at a deeper level in cells and their use of energy.
Although he pushed the boundaries in what had been impossible up until then and pioneered new and complex techniques to observe cellular actions, he got several things wrong about what those observations mean.
He published the idea that fatigue in muscles was caused by lactic acid, which in turn was caused by a lack of oxygen. People took that message and shared it with each other, changing and subtracting pieces of information and combining it with old ideas about toxic substances in the body. Thus, an industry was born.
As to what the evidence shows, Meyerhof’s idea about lactic acid began to fail very soon in scientific time—about seven years after winning the Nobel Prize. Starting with Einar Lundsgaard’s work in 1929, and continuing through many others’ research to the present, the evidence doesn’t match the predictions that the lactic acid hypothesis would imply. It turned out to be lactate instead of lactic acid, and the old ideas about massage squeezing lactic acid out of muscles as a toxin was just a story, not the reality.
As for Meyerhof, even though he was wrong about the role of lactic acid in muscle fatigue, his other work has been borne out. It laid the groundwork for needed quantitative observations and theory in cell physiology and led to understanding the roles of how cells produce energy.
It united chemistry, physics, and biology to show the integrated nature of physiology across scientific disciplines. By showing that these chemical processes work the same way in many different species, including humans, it highlights the unity and diversity of how life works.
When we make an observation of a relationship between two events or data sets, we sometimes make a mistake by indicating one of these events causes the other to happen. In other words, we see trend A associates with trend B; and so, A causes B. This is the classic correlation versus causation problem where many journalists and even scientists make when they report.
Compared to other disciplines in biology, such as genetics and evolution, research in cellular metabolism hasn’t advanced much since the Roaring Twenties. The myth stems from more than 90 years of misinterpretation of observations of an increase of lactate associated with a drop of pH level in muscle and other tissues.
Roberg, Ghiasvand, and Parker said that the term “lactic acid” is a misnomer since it was first discovered in sour milk (hence “lactic” referring to milk) by Swedish chemist Carl Wilhelm Scheele (1742–1786) in 1780. They considered the name “trivial,” yet the term—along with “lactate”—got stuck in the chemistry and medical professions for the next three centuries. Because Scheele isolated the acid under “impure conditions,” many chemists in the early 19th century tried to find alternative explanations to his findings, such as lactic acid is actually impure acetic acid.
Despite the misnomer, Robergs et al. described an early understanding of how lactic acid works in relation to exercise in the 1920s, based on the research by Meyerhof and Archibald Hill.
They highlighted that the knowledge base of acid-base chemistry and cellular respiration were “insufficient” at the time. The two chemists’ research did not directly experiment whether there was a cause-and-effect relationship between lactate and acidosis.
“…it is easy to comprehend how the Nobel prize quality of the work of Hill and [Meyerhof] was proof enough to the scientific world at that time for the interpretation that lactate production and acidosis were cause-and-effect,” Robergs et al. wrote. Hill’s studies suggest that lactic acid is the “immediate energy donor for muscle contraction,” while Meyerhof showed that lactate is a byproduct of glycogen breakdown.
Robergs et al. argued that much of the current medical education and research on lactate are still based on findings of Hill and Meyerhof’s time, which have not evolved. The idea that lactic acid and lactate are the prime contributors to lactic acidosis still permeates in modern healthcare education.
They suggested that the terms “lactate” and “lactic acid” should be “removed from any association with the cause of acidosis” in sports science, which can make coaches, trainers, athletes—and massage therapists—continue to spread the muscle soreness myth.
Like many health care myths, such as massaging a pregnant woman’s ankles can cause an abortion in her first trimester and “poor” posture is the primary cause of back pain, the lactic acid narrative may have been passed down from generations without question. The information spread so wide that even when a solid body of evidence indicates the opposite, the myth is already embedded into the culture. And it’s very difficult to change people’s minds.
Massage therapists and other manual therapists can learn from the past mistakes by keeping themselves updated and question what they learn in courses.
“Lactate can no longer be considered the usual suspect for metabolic ‘crimes’, but is instead a central player in cellular, regional and whole body metabolism.” ~ Bruce Gladden, Ph.D., Muscle Physiology Lab, Auburn University
Getting the role of lactic acid wrong was a mistake that needed correction, but it was not a fatal blow to Meyerhof’s body of scientific work. History is—and will continue to be—kind to him.