Irritable bowel syndrome (IBS) is a common condition that affects the digestive system or gastrointestinal tract. It is often a lifelong problem that requires daily symptoms management to avoid flare-ups. Both food choices and medications may be used in the treatment of IBS.
The cause of IBS is unknown but it has been attributed to stress, family history, nerve sensitivity in the gut, and motility issues as food passes through the digestive tract.
IBS pain may feel like a lot of typical gastrointestinal problems. The pain may be associated with stomach cramping, bloating, and diarrhea or constipation (typically one or the other but you can have both). You may also experience periods of flatulence, fatigue, nausea, and bathroom urgency.
Like many other conditions that affect this region of your body, IBS may also present with back pain or pelvic pain.
What is IBS?
Irritable bowel syndrome is a chronic condition that can have acute flare-ups in your guts. No one is safe from IBS as the condition affects up to 10% of individuals and has been diagnosed in children and adults of both sexes.
When diagnosed, IBS is divided into four categories:
- IBS with diarrhea
- IBS with constipation
- IBS with both diarrhea and constipation
- IBS unclassified
IBS typically starts in the second or third decade of life and is nearly twice as likely to occur in women than men. If you’re over 50 and experiencing symptoms for the first time, IBS is not likely to be the cause.
Most of its symptoms center around bowel movements. If you have the following symptoms for at least three days a month for three months or longer, you may have IBS:
- Abdominal pain and cramping
- Gas/flatulence
- Fullness
- Bloating
- Changes in bowel habits
- Frequent urination or the feeling that you are unable to empty your bladder
- Symptoms that improve or resolve after a bowel movement
Because the gastrointestinal system will appear normal on routine testing, IBS can be difficult to diagnose. Also, there is mounting evidence that IBS is not just a digestive problem. Scientists have identified changes in immune system function and how the central nervous system interprets pain as contributors to the condition.
The gut-brain connection (or axis) seems to play a role in IBS. Communication between the gut and the brain moves in both directions and is dependent on input from the neural, endocrine, and neuroimmune pathways as well. At the physiological level, the digestive system sends messages to the brain that generate responses that regulate immune function, secretion, and motility.
Simply put, this axis controls how much food you eat, digestion, and control of bowel movements. When the signals being sent along this axis are disrupted, so are the functions of your gastrointestinal system.
The types of bacteria found in the microbiome of your gut have far reaching implications. Changes in the gut microbiome can play a role in mood, behavior, stress, and anxiety. It is easy to see how a disruption of the gut-brain connection affects much more than just your abdominal region.
Can IBS cause back pain?
Both IBS and back pain are complex conditions. Similarly, we still have a lot to learn about both. Back pain is often reported in patients with IBS, but the reasons why are poorly understood. It may be referred pain (pain that starts somewhere else in the body but is felt in the back) or be linked to symptoms such as gas or bloating. The pain associated with gas and bloating has also been reported as chest pain by patients with IBS.
Individuals with IBS tend to have complex medical histories which makes sense given the connection between the gut and the immune system. IBS has been associated with other chronic illnesses such as interstitial cystitis, fibromyalgia, and rheumatoid arthritis which all share back pain as a common symptom.
IBS also seems to occur in those with chronic pelvic pain. Vulvodynia (chronic pain at the vagina opening) and testicular pain may also be symptoms of IBS. The nerve endings in the genital region are plentiful and can be irritated by excessive sitting to relieve yourself or systemic inflammation that may be part of the condition.
Interestingly, the biopsychosocial model of pain invites us to explore non-physiological sources of pain. Stress and anxiety have been linked to low back pain and to IBS via the gut-brain connection. It follows that if you are suffering from IBS which causes stress and anxiety, the physical symptom manifestation may be low back pain.
The biopsychosocial model also considers social or environmental influences on physical condition such as finances, home support, or other mental distress. These types of stresses can suppress the immune system which may lead to an IBS flare-up. Social and environmental stressors have also been associated with back pain.
Treatments for IBS and back pain
Once the diagnosis of IBS has been confirmed establishing a therapeutic alliance is of utmost importance. This is a long-term problem which makes finding a team of doctors that the patient is comfortable working with is paramount.
Patients should be educated on and encouraged to make lifestyle changes to manage their symptoms. Learning relaxation techniques such as meditation and diaphragmatic breathing can be helpful. Patients with IBS should also be encouraged to engage in regular physical activity.
Managing low back pain is never particularly easy. When it is associated with the symptoms of IBS, if you can alleviate the IBS flare-up, you should also be able to get relief for your low back pain.
Dietary changes
Dietary changes such as eating more fiber, avoiding gluten, and following the FODMAP diet may be suggested if you are diagnosed with IBS. Increasing your fiber intake can help relieve constipation by making the stool softer or provide the necessary bulk for normal bowel movements if you are suffering from diarrhea.
Increasing dietary fiber can cause gastrointestinal upset; you should gradually add fiber to your diet a little bit at a time to avoid causing gas or triggering an IBS flare-up.
Although most commonly associated with celiac disease, gluten—a protein found in wheat, barley, and rye—can also be related to IBS. A gluten elimination diet involves getting rid of cereal, grains, pasta, and many processed foods. If your symptoms improve when these foods are no longer consumed, they may be triggering your IBS.
The FODMAP diet may also be used to decrease the symptoms of IBS. The goal of the FODMAP diet is to reduce or eliminate foods that contain carbohydrates. Symptoms may improve when these foods are avoided because they are difficult to digest. FODMAP foods include:
- Fresh fruits (apples, blackberries, cherries, nectarines, peaches, watermelon, etc.) and their juices
- Canned fruits, fruit juices, or dried fruits
- Vegetables (artichokes, asparagus, cabbage, cauliflower, garlic, mushrooms, onions, and peas)
- Lentils and beans
- Dairy products
- Wheat and rye
- Honey and foods with high-fructose corn syrup
- Products containing “fake” sugars such as sorbitol, mannitol, xylitol, and maltitol (commonly found in candy, mints, and gum)
Probiotics
For the most part, probiotics can help manage the symptoms of IBS. Probiotics are antimicrobial which makes them protective against pathogenic bacteria. Probiotics can also help enhance the barrier created by the intestinal wall and make it less likely that bacteria will leak out (leaky gut syndrome) and reduce the hypersensitivity of the abdominal organs seen in those with IBS.
A meta-analysis performed by the American College of Gastroenterology found that probiotics were helpful in reducing overall symptoms as well as gas and bloating in patients with IBS.
Bifidobacterium and lactobacillus seem to be the most helpful probiotics if you have IBS. Even in their inactive form, probiotics can still be beneficial.
One note of caution: if you also suffer from SIBO (small intestinal bacterial overgrowth) probiotics can make the overgrowth worse and magnify symptoms.
Exercise
Research has shown that patients who perform regular physical activity three to five days a week for three months had a reduction in both IBS symptoms and psychological symptoms.
Another study also showed that yoga was an effective means of reducing the severity of IBS symptoms and that simply walking improved overall abdominal symptoms, mood, and anxiety.
In fact, exercise may be the most effective long-term treatment approach if you have IBS. A 2015 study followed up with patients at an average of five years out. Not only did these patients have overall improvement IBS symptoms but also psychological symptoms, such as fatigue, depression, anxiety, and quality of life.
Stress management
Exercise has also been shown to help with overall stress management. Low-impact, cyclical activities such walking, swimming and cycling can reduce stress. These activities may also help your bowels contract and relax normally rather than the overreaction that is characteristic of IBS.
Taking up activities that strengthen the mind-body connection or focus on mindfulness can also be a tool for managing your symptoms. Meditation, relaxation, qi gong, diaphragmatic breathing, tai chi and yoga are just a few options.
One of the great things about the internet is how easy it is to find a creator who wants to share their content with you. YouTube is an excellent resource for videos on meditation, yoga, relaxation breathing, and all things mindfulness.
Medication
The goal of pharmaceutical management of IBS is to address the pain and discomfort in the abdomen and the changes in bowel habits. Several types of medications may be employed in the management of IBS.
- Laxatives to improve constipation
- Antidiarrheals to improve diarrhea
- Secretagogues/prosecretory agents to help alleviate pain, discomfort and bloating
- Retainagogues to block the absorption of sodium which can draw water into the intestinal tract to create softer stool, speed up intestinal transit time, and address pain and bloating
- Antispasmodics to decrease smooth muscle contraction of the intestines and decrease the pain and discomfort from abdominal cramping
- Antidepressants or neuromodulators to impact the signals (increase or decrease) in the brain-gut connection
- Antibiotics to modify bacteria in the gut and act as an anti-inflammatory agent
- Serotonin agonists/antagonists to address gut secretion, movement of food through the intestines, and sensation.
Other therapies still being investigated include bile-acid binding, fecal transplants, and cannabinoids.
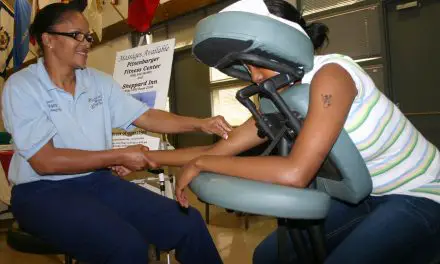
Massage therapy
Massage therapy, including self-massage, can be useful in managing your IBS. It has been shown to have several effects on the gastrointestinal system which can help alleviate the symptoms of IBS.
Gentle abdominal massage can help with the mind-body connection by activating the parasympathetic nervous system (“rest and digest”) and decreasing hypersensitivity of the abdominal organs.
If you’re in the throes of a flare-up, massage should avoid direct compression of the abdomen. This may mean the work is done side-lying rather than on your stomach, depending on your tolerance to positioning. Massage to the low back- gentle or using deeper strokes- can also help alleviate the pain associated with IBS.
Getting help for IBS and back pain
An occasional stomach ache isn’t likely cause for concern but when that stomach ache becomes a regular occurrence it may be time to see your physician. This is especially true if you regularly experience constipation, diarrhea, and abdominal pain.
A diagnosis will typically be made based on your description of symptoms (duration, frequency, intensity, etc.). Abdominal pain that occurs an average of once a week for 12 weeks and is associated with changes in bowel movements is typically classified as IBS.
Irritable bowel syndrome is a diagnosis of exclusion. There’s no specific test for IBS, but your physician may order blood tests, stool tests, a pelvic exam, or other testing to rule out other conditions.
Resources
About Irritable Bowel Syndrome (IBS)
American College of Gastroenterology: Irritable Bowel Syndrome
American Gastroenterological Association: irritable Bowel Syndrome (IBS)

Penny Goldberg, DPT, ATC
Penny Goldberg, DPT, ATC earned her doctorate in Physical Therapy from the University of Saint Augustine and completed a credentialed sports residency at the University of Florida. She is a Board Certified Clinical Specialist in Sports Physical Therapy.
Penny holds a B.S. in Kinesiology and a M.A. in Physical Education from San Diego State University. She has served as an Athletic Trainer at USD, CSUN, and Butler University.
She has presented on Kinesiophobia and differential diagnosis in complicated cases. Penny has published on returning to sports after ACL reconstruction and fear of movement and re-injury.
Outside of the clinic, Penny enjoys traveling, good cooking with great wine, concerts, working out and playing with her dogs.