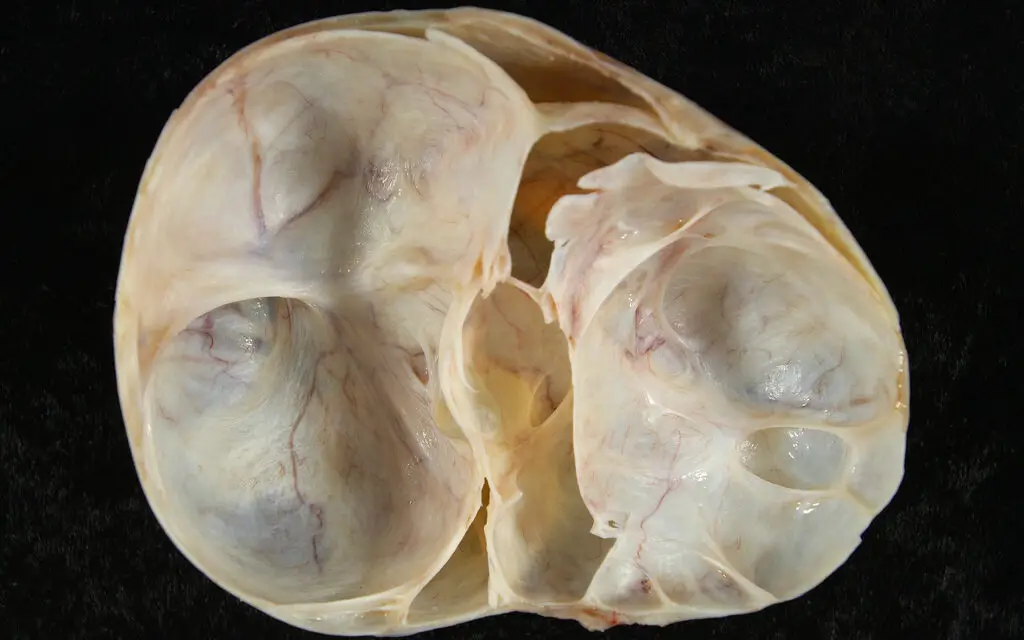
Ovarian cysts are fluid-filled sacs found in or on the surface of an ovary. These cysts are a relatively common among those with a uterus of child-bearing age. There are many different kinds of ovarian cysts but most are caused by a normal menstrual cycle. The cysts develop when the ovarian follicles keep growing instead of releasing eggs during ovulation.
The risk of developing an ovarian cyst can be higher if you:
- take fertility drugs
- are currently pregnant
- have a history of endometriosis
- have severe pelvic infection
- previously have had a cyst
Ovarian cysts are mostly harmless other than causing pelvic pain, bloating, abdominal discomfort, and low back pain, but some can be asymptomatic. For those that do cause symptoms, finding ways to relax, such as a hot bath or heating pad. can help alleviate pain or discomfort.
Ovarian cysts and back pain
Most ovarian cysts do not require treatment and may even go unnoticed. Larger ovarian cysts may start to impede the space in your abdomen which can put abnormal pressure on your organs. In the case of a large, space-occupying cyst, you may develop a deep, dull, aching type of lower back pain.
There are dozens (if not hundreds) of causes of low back pain. It’s important to consider the entire clinical picture when determining the cause of your back pain. High stress levels, poor postural awareness, and disc injury have all been associated with low back pain too.
Types of ovarian cysts
There are several types of ovarian cysts, which can range in size from just a few centimeters to more than a foot long.
Functional cysts
Functional cysts are almost always harmless and typically resolve on their own in a month or two. These form naturally as part of a normal menstrual cycle. In the stages that lead up to ovulation, small follicles grow in your ovaries. These follicles are responsible for hormone release and expulsion of the egg ovulation. When a normal follicle continues growing and holding fluid after the menstrual cycle, a functional cyst forms.
Endometriotic cysts
Endometriotic cysts are caused by endometriosis. During the menstrual cycle, your body releases hormones that cause the uterine tissue to be shed and expelled after ovulation. When endometrial tissue forms outside of the uterus (as in endometriosis) on the ovaries, it cannot be shed. This tissue builds up and forms dark, reddish brown endometriosis cysts (sometimes called “chocolate cysts”). These cysts tend to need medical attention as they do not heal on their own. Rupture of these cysts can cause pelvic pain, scar tissue or adhesions, and infertility.
Benign neoplastic cysts
Benign neoplastic cysts are a rare variety and are described by their abnormal tissue growth. Benign neoplastic cysts can take on many forms as they can be made up of any collection of cells:
Cystic teratoma or dermoid cyst
These cysts develop from germ cells and can be made up of multiple tissue types (sebaceous glands, skin cells, or hair follicles). These cysts may or may not cause symptoms, but when they do, they can cause pelvic pain and typically require some sort of medical treatment.
Although most ovarian cysts are benign, any cyst can become cancerous or malignant. Tumors, or malignant cysts, are an indication of ovarian cancer. If you’re experiencing unexplained weight loss or weight gain, fever or night sweats, or unexplained pelvic pain or symptoms, you should seek advice from your physician.
What causes ovarian cysts?
Most ovarian cysts form as part of the normal menstrual cycle. Follicles, or small cysts, are formed every month by the ovaries. When this follicle keeps growing, it’s called a functional cyst.
Functional cysts can be further divided into follicular cysts and corpus luteum cysts. In normal menstruation, about halfway through your cycle, the egg bursts out of the follicle and continues its travels down the fallopian tube. If the follicle doesn’t rupture, the egg remains inside while the follicle continues to grow and a cyst is formed.
Corpus luteum cysts can be formed after the follicle releases the egg. In normal menstruation, the follicle then shrinks and produces estrogen and progesterone which are the hormones needed for conception. At this point, the follicle becomes the corpus luteum. When the opening where the egg comes out of is blocked, fluid can build up inside the corpus luteum and cause a cyst to be formed.
The risk factors for ovarian cysts include:
- Infertility treatments
- Tamoxifen (hormone therapy used in the treatment of breast cancer)
- Pregnancy
- Hypothyroidism
- Smoking
- Tubal ligation
Ovarian cyst treatments
Ovarian cysts can be detected during a pelvic exam or with imaging. The size of the cyst, contents of the cyst (fluid vs. solid), age, and menopausal status can all effect if and how the cyst should be treated.
Some of the tests used to identify ovarian cysts are: pregnancy tests, ultrasound, laparoscopy, and tumor marker tests.
Your age, the size of the cyst, and your symptoms all play a major role in determining which treatment path is right for you.
Wait and see
Most of the time, it is safe to take a “wait and see” approach to treatment of ovarian cysts. Most cysts have disappeared by the time reexamination occurs. If you have no symptoms but cysts are identified with pelvic ultrasound, this will typically be the recommended treatment. You may need to have multiple follow-up ultrasounds to watch for changes in the size of the cyst.
Medication
The goal of contraceptive medicine is to keep you from ovulating (and thus becoming pregnant).Using contraceptives such as birth control pills can prevent you from developing ovarian cysts. If you already have a cyst, this type of medication is not a treatment option as it will not shrink and already present cyst.
Surgery
A large cyst that looks out of the ordinary might require surgical removal. Tumors that are painful or continuing to grow might also need surgery. It is possible to spare the ovary when removing the cyst in some cases.
Complications of ovarian cysts
There are three main complications that are common with ovarian cysts. They are rupture, hemorrhage, and torsion.
A cyst that ruptures, or bursts open, can cause serious problems. Ruptured cysts can cause severe pain and bleeding (hemorrhage). Bigger cysts are more likely to rupture. This can cause pain into your low back or thighs. If you currently have a cyst, vigorous activity that involves the pelvis, such as sexual intercourse, can increase the chance that the cyst ruptures.
One of the leading causes of gynecological emergency department visits is ovarian torsion. In ovarian torsion, a large cyst causes the ovary to move which can create the painful twisting (or torsion) of the organ. If you have ovarian torsion, you may experience sudden, severe pain in the pelvis or low back along with nausea and vomiting. This can become a medical emergency if blood flow to the ovary is reduced or stopped.
Does exercise help reduce ovarian cysts?
If you’re experiencing a symptomatic ovarian cyst, activity modification may be the first step in your treatment. Strenuous physical activity, including vaginal sex, can cause pain in the pelvis or low back when cysts are present.
On the other hand, light to moderate exercises may help manage the symptoms of a cyst. Exercise that decreases stress (and thus the release of stress hormones) or helps you maintain a healthy body weight can keep the symptoms associated with ovarian cysts at bay.
In the early stages of symptoms, exercise may help you and your physician differentiate musculoskeletal low back pain from something more sinister. Low back pain that is muscular in origin tends to improve quickly with movement. Low back pain that has a more systemic cause, may not change with exercise or movement.
If you have been diagnosed with polycystic ovary syndrome (PCOS), a condition where the menstrual cycle is no longer regular and cysts form consistently, exercise may be part of your treatment plan as well. The complications of PCOS are obesity and infertility, both of which are helped by exercise.
If you have been diagnosed with PCOS, exercise can help with hormone regulation. Exercise creates hormonal changes, combats obesity and metabolic syndrome, reduces inflammation, and increases immunity.
Getting help
If you’re experiencing sudden, severe pain in your abdomen or pelvis, fever or vomiting, or signs of shock, you should seek immediate medical attention as these should be signs of a ruptured cyst or hemorrhaging.
In non-emergent situations, you can expect your physician to perform a pelvic exam as well as manual pressure over the areas in your abdomen where a cyst could form. If indicated, your physician may refer you to a lab or other facility for follow-up testing including blood tests, pelvic ultrasound, laparoscopy.
Resources
Ovarian Cancer Research Alliance: Ovarian Cysts
American College of Obstetricians and Gynecologists: Ovarian Cysts
U.S. Department of Health & Human Services: Office on Women’s Health

Penny Goldberg, DPT, ATC
Penny Goldberg, DPT, ATC earned her doctorate in Physical Therapy from the University of Saint Augustine and completed a credentialed sports residency at the University of Florida. She is a Board Certified Clinical Specialist in Sports Physical Therapy.
Penny holds a B.S. in Kinesiology and a M.A. in Physical Education from San Diego State University. She has served as an Athletic Trainer at USD, CSUN, and Butler University.
She has presented on Kinesiophobia and differential diagnosis in complicated cases. Penny has published on returning to sports after ACL reconstruction and fear of movement and re-injury.
Outside of the clinic, Penny enjoys traveling, good cooking with great wine, concerts, working out and playing with her dogs.