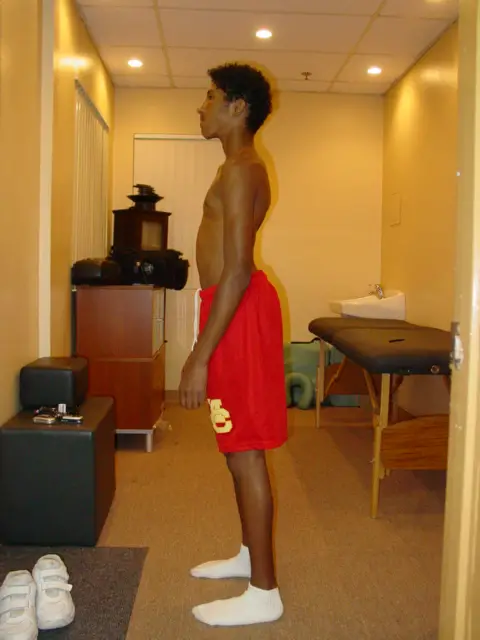
Pelvic tilts and bony landmarks vary among many pain-free individuals, yet why so many clinicians try to “fix” patients’ posture?
A recent systematic review of non-surgical treatments for the anterior pelvic tilt had brought up some discussions on social media regarding how reliable is the assessment of pelvic tilts among patients with back pain. (1)
The researchers Brekke et al.,said, “No evidence supports excessive anterior pelvic tilt as an isolated clinical disorder or pathology,” and having a cutoff point in determining what an excessive pelvic tilt means can be misleading because “sagittal balance can be individually regulated to maintain a proper posture.” (1)
In other words, each person has their own way to move and adapt, and no single range of anterior pelvic tilt can fit into everyone’s movement patterns and body.
“Looking for pelvic tilts is subjective, not to mention that postural adjustments are made moment to moment. The accuracy of assessing a tilt is not reliable nor is it functional,” Dr. Susie Gronski said in an email interview, who is a pelvic pain physical therapist practicing in Asheville, North Carolina.
“There is an overwhelming amount of evidence to sway my bias in the direction that tissue-based issues are not the sole factor in someone’s pain experience. Of course, peripheral nociception can be one factor for tissue sensitivity, but [it is] not the only factor at play.”
Gronski also said that pain “is a conscious experience that motivates us to take action, grabs our attention.”
“Nociception involves peripheral sensory neurons picking up on changes in the tissue environment and sending these messages to the spinal cord and brain,” Gronski said. “The brain filters the information and whether someone will experience pain or not is highly dependent on context, their beliefs and thoughts about pain, and even subconscious factors that we have yet to discover.”
What does current research say about pelvic tilt assessments?
Research in pelvic anatomy and posture finds some factors that can cause clinicians to make false positive findings in pelvic tilt assessments. A 2005 study of 160 pain-free subjects from a medical center in Lyon, France, found a wide range of pelvic and spinal postural variations.
For example, the S1 joint had a variation between 20 to 65 degrees at the vertebral endplate at the horizontal axis, and lumbar lordosis varied between 41 to 82 degrees. (2)
An earlier study in 1982 also found similar variations among 100 asymptomatic samples. The researchers, led by the late Dr. Pierre Stagnara, said that it is “unreasonable to speak of normal kyphosis and lordotic curves” because their data found a wide range of curvatures. “The average values are only indicative and not normative. The extreme values show the morphologic latitude of the human species.” (3)
Even the landmarks that clinicians were taught to palpate in a pelvic tilt assessment—anterior superior iliac spine (ASIS) and posterior superior iliac spine (PSIS)— vary in position and angle.
One British study, led by Dr. Stephen Preece from the University of Salford, compared the angles of the ASIS and PSIS of 30 pelvises and found a wide variation (0 to 23 degrees). The researchers also found variation in the angles from the ischial tuberosity to the iliac crest on both sides of the pelvis. (4)
They warned, “The ASIS-PSIS angle should not be used in isolation to assess pelvic orientation. Additional factors should also be taken into consideration, such as the depth of the lumbar lordosis and the hip joint angle in standing with neutral knee joint alignment.” Any type of pelvic tilt assessment should be “viewed with caution.” (4)
However, a previous larger study of 323 radiographs of the pelvis found a similar pattern of asymmetry between the left and right sides of the pelvis where the researchers measured the difference of heights from the iliac crests to the acetabuli. (5) They reported “a much lower prevalence and a smaller range of pelvic asymmetries” compared to earlier similar studies. (6) The primary difference is that this study included scans of the pelvis and abdominal region, not just from scans of patients with back pain, and it did not included ASIS-PSIS angles.
“To say that any one body needs to be in any one posture or position is unrealistic, fear-mongering, and steals a person’s self-efficacy by sending messages of fragility instead of capability.” ~ Dr. Susie Gronski
Is pelvic tilt posture assessment a waste of time?
Maybe, and maybe not. This is a debatable subject with no definitive agreement yet among a variety of healthcare professionals. However, given that pain is a multi-factorial subjective experience and the current scientific literature find a weak correlation of posture and pain, clinicians should not narrow the cause down to one factor. There is no need to be obsessive with anatomical landmarks when there are likely other factors that contribute to each patients’ pain.
Gronski asked three questions to clinicians who do use pelvic tilt assessment: Why are you assessing? What valuable information does it provide? How does it translate into function or helping that person move better?
For example, physical therapists use certain hands-on tests to see if there is pain or dysfunction in a patient’s sacroiliac joint. Although such tests are able to differentiate pain between the lower back and sacroiliac joint, they do not tell clinicians or patients why there is pain.
“These tests also tell us nothing about the amount of movement in the sacroiliac joint,” Gronski said. “In fact, the reliability of feeling a few degrees of motion in a structure that is very stable and support is questionable. We’re talking about millimeters of movement.”
Gronski added that pelvic tilt assessments “rarely translate to any real changes in someone’s ability to function in life, do what they love, or eliminate their pain.”
“To say that any one body needs to be in any one posture or position is unrealistic, fear-mongering, and steals a person’s self-efficacy by sending messages of fragility instead of capability,” she said.
If pelvic tilts were a reliable factor to determine a cause-and-effort relationship between posture and pain, research in the past 40-plus years would have found a consistent pattern in how people with back pain or hip pain would have different postures than those without pain. Pain-free subjects would exhibit a consistent postural pattern compared to symptomatic subjects when other factors are controlled for, such as gender and age.
Perhaps a better solution would be to encourage patients to tell their story about their pain. This allows both the clinician and the patient to explore other possibilities of why the pain exists and let the clinician to have a better insight of the patient’s problem beyond their biology.
“It’s important to approach pain care that is person-centered rather than symptom centered,” Gronski said.
References
1. Falk Brekke A, Overgaard S, Hróbjartsson A, Holsgaard-Larsen A. Non-surgical interventions for excessive anterior pelvic tilt in symptomatic and non-symptomatic adults: a systematic review. EFORT Open Rev. 2020;5(1):37–45. Published 2020 Jan 29. doi:10.1302/2058-5241.5.190017.
2. Roussouly P, Gollogly S, Berthonnaud E, Dimnet J. Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine (Phila Pa 1976). 2005 Feb 1;30(3):346-53.
3. Stagnara P, De Mauroy JC, Dran G, Gonon GP, Costanzo G, Dimnet J, Pasquet A. Reciprocal angulation of vertebral bodies in a sagittal plane: approach to references for the evaluation of kyphosis and lordosis. Spine (Phila Pa 1976). 1982 Jul-Aug;7(4):335-42.
4. Preece SJ, Willan P, Nester CJ, Graham-Smith P, Herrington L, Bowker P. Variation in pelvic morphology may prevent the identification of anterior pelvic tilt. J Man Manip Ther. 2008;16(2):113–117. doi:10.1179/106698108790818459
5. Badii M, Shin S, Torreggiani WC, Jankovic B, Gustafson P, Munk PL, Esdaile JM. Pelvic bone asymmetry in 323 study participants receiving abdominal CT scans. Spine (Phila Pa 1976). 2003 Jun 15;28(12):1335-9.
6. Ingelmark E, Lindstrom J. Asymmetries of the lower extremities and pelvis and their relations to lumbar scoliosis. Acta Morphol Neerl Scand. 1963;5:221–34.
7. Clarke GR. Unequal leg length: an accurate method of detection and some clinical results. Rheumatol Phys Med 1972;11:385–90.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.