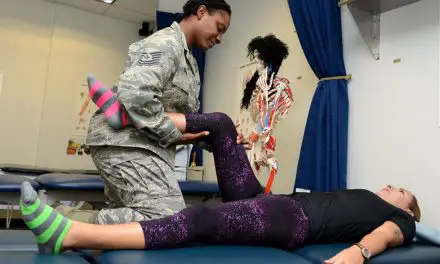
Imagine being a child in the hospital with several weeks of treatment ahead of you before you can go home. Doctors and nurses enter your room multiple times a day, dressed in isolation gowns, gloves, and masks. They visit you about your medication, progress, and upcoming procedures.
Then they leave.
During some visits, someone takes your blood or checks your vital signs.
Picture now a different caregiver entering your room. This person is also gowned, but she is here to give your aching body a therapeutic massage.
I have been a massage therapist for 12 years and a pediatric massage therapist for five years. For the past year and a half, I have been providing massage therapy for hospitalized children at Cook Children’s Medical Center in Fort Worth, Texas.
I received my pediatric training with Tina Allen of Liddlekidz, which focused on providing massage therapy for children with special healthcare needs, children who are hospitalized or have been diagnosed with a terminal illness in hospice care.
I work within the pain management program at Cook Children’s, which is an acute and chronic pain service that focuses on the multidisciplinary aspects of managing pain.

Photo by William Fortunato.
The pain department philosophy is that pain is a complex disease process that not only involves organic causes of pain but also the individual’s own experience of pain. The most effective way to manage pain is through a multi-modal approach.
I work with children with varied physical, developmental, emotional and mental challenges. I see patients throughout the entire hospital and am consulted by nearly every department including hematology/oncology, pain management, neurology, cardiology, orthopedics, pulmonology, nephrology, hospitalists, and critical care.
I also work closely with physical therapy and occupational therapy. Even though I work within the pain management department, massage can be ordered without a pain consult.
When a physician order is received, it may or may not have a specific issue to address or any restrictions listed. Before seeing the patient, I read the patient’s chart for a complete health history, diagnosis, reason for admission, physician reports and nursing notes for information that may affect treatment parameters.
I also check to see if procedures or testing are ordered which affect when I can see the patient. If I have any questions or concerns not addressed in the chart, I will speak with the bedside nurse.
When I first meet a patient, I introduce myself to them and their parent and explain what I can offer. Consent from the parent and permission from the patient are needed prior to the massage.
In most instances, the family and patient are expecting me because their provider has already talked to them about massage therapy services. The patient treatment plan is determined by the patient’s needs and desires.
I had a 13-year-old boy who was diagnosed with high risk AML (acute myeloid leukemia). He was going through intense chemotherapy in hopes of getting him into remission for a bone marrow transplant. He had leg and feet pain that his physician thought massage therapy would be beneficial. He was sick and cranky and not too excited about someone touching him.
His mother talked him into it saying “Your doctor wants you to try this.” I let him know that we would stop if he didn’t like it. Shortly after starting his massage, he let out a big sigh.
I asked him if he was okay and he replied “This feels so good.” I continued giving him daily massages through chemotherapy and through his bone marrow transplant.
I often have a patient who is non-verbal due to age, injury, or disease. Being aware and responsive to engagement cues is important. Family members are most helpful in interpreting their child’s needs in these incidents.
Patient monitors are useful cues; I have had nurses wait until after a patient’s massage to administer medications (but obviously not during a lifesaving situation). On a few situations, medication was deferred.
I have so many stories from the last 18 months. I love children. I have been comfortable around “sick people” since I was a child. Pain and suffering is complex, massage and comforting is not. I have journeyed with children to healing and I’ve taken some to the end.